Hand Therapy
Hand therapy is part of the role of an occupational therapist. It is our priority to make sure our clients leave us while being able to run an independent life. The hand is an important organ in the body that allows the client to engage in daily life activities such as writing. While we are focusing mainly on hand treatment, it is important to not lose sight that we as occupational therapists should engage and build a rapport with our clients and keep them motivated during therapy. We need to make sure not to focus only on hand treatment but to get a wider understanding about their life and what motivates them, they should know how their treatment helps to bolster recovery and what they need to have an independent life.

The anatomy of the hand is extraordinarily complex and is composed of many different bones, muscles, and ligaments that allow for the majority of movement and dexterity. Contained within the hand are three major types of bones: carpal bones, metacarpals, and phalanges. Whereas the wrist contains eight bones: the two rows of carpal bones (Scaphoid, Lunate, Triquetrum, and Pisiform) that are connected to two bones located in the arm, the ulna bone, and the radius bone. The second row (Trapezium, Trapezoid, Capitate, and Hamate) connects to the metacarpal bones. The metacarpal bones consist of 5 different bones that make up the middle part of the hand that connects to the phalanges. Within the fingers, there are fourteen bones in each hand and also in the toes of each foot. Each finger has three phalanges (the distal, middle, and proximal); unlike the thumb which only has two (the proximal and distal).
Numerous muscles, ligaments, tendons, and sheaths can be found within the hand. The muscles act as structures that can contract, allowing movement of the bones in the hand. The ligaments are composed of fibrous tissues that help bind together all the joints in the hand. The sheaths are tubular structures that surround part of the fingers and the tendons connect the muscles in the arm of hand to the bone which allows movement to occur. In addition, there are arteries, veins and nerves within the hand that provide blood flow and sensations to the hand and fingers.



There are four joints in each finger totaling twenty joints in each hand, in addition, there is the distal radioulnar joint which allows for the rotation of the hand at the wrist point. Hand pain is often the result of a recent injury or from overusing the hand or wrist (mentioning all the joints)
Finger joints
Thumb
-
Interphalangeal Joint (IP)
-
Metacarpophalangeal Joint (MP)
-
Carpometacarpal Joint (CMC)
Fingers little to index finger
-
Distal Interphalangeal Joint (DIP)
-
Proximal Interphalangeal Joint (PIP Joint)
-
Metacarpophalangeal Joint (MCP joint)
-
Carpometacarpal Joint (CMC Joint)
Wrist joints
-
Radiocarpal joint
-
Ulnocarpal joint
-
Distal radiocarpal joint

Ligaments of the wrist
-
Palmar radiocarpal: located in the anterior side of the hand. It passes from the radius to both rows of carpal bones.
Function: increasing stability, supination of the forearm.
-
Dorsal radiocarpal – located in the posterior side of the hand. It passes from the radius to both rows of carpal bones.
Function: stability of the wrist, pronation of the forearm.
-
Ulnar collateral – passes from the ulnar styloid process to the triquetrum and pisiform.
Function: support the collateral ligament to prevent excessive lateral joint displacement.
-
Radial collateral – passes from the radial styloid process to the scaphoid and trapezium.
Function support collateral ligament to prevent excessive lateral joint displacement.
-
Triangular fibrocartilage complex (TFCC): a cartilage structure located on the small finger side of the wrist that is formed by the triangular fibrocartilage discus (TFC), the radioulnar ligaments (RULs) and the ulnocarpal ligaments (UCLs).
It cushions and supports the small carpal bones in the wrist. The TFCC keeps the forearm bones (radius and ulna) stable when the hand grasps or the forearm rotates.
ligament of the finger (IPs Joints): -
-
Collateral ligaments found at the sides of each interphalangeal joint, originating from proximal phalanx and extending to the palmar, or volar side of the hand.
Accessory ligament for collateral ligament arises from each side and extends anteriorly to attach to the fibers of the palmar ligament.
Function: help to prevent excessive adduction-abduction movements of the interphalangeal joints.
-
(Palmar/Volar plates) Ligament: located on the palmar surface of each interphalangeal joint with its distal part arching across the base of the distally lying phalanx to blend with the accessory collateral ligaments.
Function: prevent excessive hyperextension of the joint
There are two types of muscles that cover the hand. The extrinsic muscles, which originate from the arm and insert into the wrist, and the intrinsic muscles, which originate and insert into the wrist. The intrinsic muscles of the hand are divided into three groups: the thenar, hypothenar, and intermediate muscles according to the location of the wrist. (mentioning all the muscles)
Extrinsic Hand muscles:



Intrinsic Hand Muscles:

Wrist Flexors
Flexor Carpi Ulnaris
-
Origin: Common flexor origin – (Medial epicondyle) •
-
Insertion: Base of 5th metacarpal, and pisiform bone.
-
Innervation: Ulnar nerve
-
Action: Wrist flexion/ Ulnar deviation
Flexor carpi radialis
-
Origin: Common flexor origin – (Medial epicondyle)
-
Insertion: Base of 2nd metacarpal
-
Innervation: median nerve
-
Action: Wrist flexion/ Radial deviation
Wrist Extensors
Extensor Carpi Ulnaris
-
Origin: Common extensor origin. – (Lateral epicondyle)
-
Insertion: Base of 5th metacarpal.
-
Innervation: Radial nerve. – Posterior interosseous nerve A deep motor branch of the Radial nerve
-
Action: Wrist Extension/ Ulnar deviation
Extensor Carpi Radialis Longus
-
Origin: Common extensor origin – (Lateral epicondyle)
-
Insertion: Base of 2nd metacarpal
-
Innervation: Radial nerve
-
Action: Wrist extension/ Radial deviation
Extensor Carpi Radialis Brevis
-
Origin: Common extensor origin – (Lateral epicondyle)
-
Insertion: Base of 3rd metacarpal
-
Innervation: Radial nerve – Posterior interosseous nerve
-
Action: Wrist extension/ Radial deviation
Fingers Flexors
Flexor Digitorum Superficialis (FDS)
-
Origin: Common flexor origin – And proximal half of radius
-
Insertion: Middle phalanges of digits 2-5 – Each digit of FDS has a separate muscle belly
-
Innervation: Median nerve
-
Action: Flexes PIP joints
Flexor Digitorum Profundus (FDP)
-
Origin: proximal two-third of Ulna (anterior and median side)
-
Inserstion: distal phalanx of digit 2-5
-
Innervation:
-
median nerve (index and long finger)
-
Ulnar nerve for (ring and little finger)
-
-
Action: flex the DIP
Finger Extensor
Extensor Digitorum Communis
-
Origin: Common extensor origin
-
Insertion: Extensor mechanism– Dorsal Surface of distal & middle phalanges.
-
Innervation: Radial nerve – Posterior interosseous nerve
-
Action: Finger MCP & IPs Extension
Extensor Indicis
-
Origin: Posterior surface of ulna – Lower 1⁄2
-
Insertion: Extensor mechanism of 2nd digit
-
Innervation: Radial nerve – Posterior interosseous nerve
-
Action: Extends 2nd digit
Extensor Digiti Minimi
-
Origin: Common extensor origin
-
Insertion: Extensor mechanism of 5th digit
-
Innervation: Radial nerve – Posterior interosseous nerve
-
Action: Extends 5th digit
Thenar Extrinsic muscles (Thumb)
Flexor Pollicis Longus (FPL)
-
Origin: Anterior middle 1⁄2 of radius
-
Insertion: Base of distal phalanx of the thumb
-
Innervation: Median nerve – Anterior interosseous
-
Action: Thumb IP Flexion
Extensor Pollicis Longus
-
Origin: Dorsal ulna
-
Insertion: Base of distal phalanx – Posterior side
-
Innervation: Radial – Posterior interosseous
-
Action: Thumb IP Extension
Extensor Pollicis Brevis
Origin: Dorsal of radius
-
Insertion: Base of proximal phalanx – Posterior side
-
Innervation: Radial – Posterior interosseous
-
Action: Thumb MCP Extension
Abductor Pollicis Longus
-
Origin: Posterior ulna (proximal) – Posterior distal radius
-
Insertion: Base of first metacarpal
-
Innervation: Radial – Posterior interosseous
-
Action: Thumb CMC Abduction


Intrinsic muscles of the hand Thenar
Flexor pollicis brevis
-
Origin – Superficial head – trapezium– Deep head – trapezoid & capitate
-
Insertion: Base of proximal phalanx
-
Innervation: – Superficial – median – Deep – Ulnar
-
Action: Thumb MCP Flexion
Abductor pollicis brevis
-
Origin: Scaphoid & Trapezium – Transverse carpal ligament
-
Insertion: Base of proximal phalanx
-
Innervation: Median
-
Action: Thumb CMC Abduction
Adductor pollicis
-
Origin: – Oblique Head: Capitate bone – Transverse Head: 3rd metacarpal
-
Insertion: Base of proximal phalanx (ulnar side)
-
Innervation: Ulnar
-
Action: Thumb Adduction
Opponens pollicis
-
Origin: Trapezium – Transverse Carpal Ligament
-
Insertion: Shaft of 1st metacarpal
-
Innervation: Median
-
Action: Thumb Opposition – MCP flexion, abduction & rotation
intermediate
Dorsal Interossei (abductors)
-
Origin: Side of metacarpals – 1st & 2nd radial side – 3rd & 4th ulnar side
-
Insertion: Extensor
-
mechanism
-
Innervation: Ulnar nerve
-
Action: MCP Abduction
Palmar Interossei (adductors)
-
Origin: Base of metacarpals of 2, 4 & 5th digits.
-
Insertion: Extensor mechanism
-
Innervation: Ulnar nerve
-
Action: MCP Adduction
Lumbricals
-
Origin: Tendons of FDP
-
Insertion: Extensor expansion – Dorsal aspect of 2-5 digits, radial side.
-
Innervation: – 1 & 2 – median – 3 & 4 – ulnar
-
Action:
-
MCP flexion 2-5 digits
-
DIP & PIP ext 2-5 digits
-
hypothenar
Abductor Digiti Minimi
-
Origin: Pisiform
-
Insertion: Base of 5th proximal phalanx – Ulnar side
-
Innervation: Ulnar
-
Action: Abduction of 5th digit
Opponens Digiti Minimi
-
Origin: Hook of hamate – Transverse carpal ligament
-
Insertion: Ulnar border of entire 5th metacarpal bone
-
Innervation: Ulnar
-
Action: Little finger opposition
Flexor Digiti minmi
-
Origin: hook of hamate – medial aspect of flexor retinaculum
-
Insertion: medial side of the base of proximal phalanx of the little finger.
-
Innervation: ulnar nerve
-
Action: flex the fifth / opposition of the little finger.


-
Cumulative Trauma Disorder (CTD) Nerve Entrapment: is a mechanism of injury, not a diagnosis. its also called Repetitive strain injury (RSI)
Median Nerve
Carpal Tunnel Syndrome
How to test it: (click on the test for more information)
-
Hold the wrist flexed at 90 degrees for 1 minute, it will result in Tingling or numbness
-
tap on lightly over the patient transverse carpal ligament,
-
MMT: abductor pollicis Brevis (weakness)
Pronator Teres Syndrome
Anterior interosseous syndrome
Ulnar Nerve
Ulnar Tunnel Syndrome
How to test it
-
Muscle wasting
-
-
Wartenberg’s sign (5th finger is abducted)
-
Cubital Tunnel Syndrome
-
-
-
Wartenberg’s sign (little finger abducted)
-
Hold elbow in flexion for 5 min = (Numbness in ulnar nerve distribution/ Pain in the forearm/ Wasting or weakness of intrinsic hand muscles)
Symptoms include: Tenderness/ Pain/ Swelling
-
DeQuervain's tenosynovitis —the most common type of tenosynovitis disorder. It causes pain and swelling in the tendon sheath in the thumb. Inflammation of the first
dorsal compartment affects the APL & EPB. Located in the Radial border of the anatomic snuffbox
Caused by repetitive hand and thumb motions such as:
-
Grasping
-
Pinching
-
Squeezing
-
Repetitive ulnar deviation
Thumb adducted in the palm, Ulnar deviation of the wrist, Pain radiates from the first dorsal compartment
-
Trigger finger or trigger thumb—a type of tenosynovitis where the tendon sheath becomes inflamed and thickened making it hard to bend or straighten the finger or thumb. The finger or thumb may lock or "trigger" suddenly and the tendon becomes unable to smoothly glide within the sheath. (In Kuwait, it's most common between females). Typically occurs in the first annular pulley (A1)
-
Grading for trigger finger
-
Grade I Palm pain and tenderness at A-1 pulley
-
Grade II Catching of digit
-
Grade III Locking of digit, passively correctable
-
Grade IV Fixed, locked digit
-

what are the flexor pulley?
The flexor pulley system of the hand is a complex structure that co-ordinates flexion of the digits. It holds the flexor tendons against the phalanges; preventing them from pulling away and (bowstringing: action is seen, in which the affected finger fails to flex fully and is associated with pain or discomfort). This allows efficient flexion of the individual digits by the long flexor muscles
Long flexor tendons – and their associated synovial sheaths.
Annular pulleys: 5 associated with each finger, 2 associated with the thumb.
-
A1: overlies the metacarpophalangeal joint
-
A2: overlies the proximal aspect of the proximal phalanx
-
A3: overlies the proximal interphalangeal joint
-
A4: overlies the mid-portion of the middle phalanx
-
A5: overlies the distal interphalangeal joint
-
A2 and A4 most important pully because they prevent bowstringing
Cruciate pulleys – 3 associated with each finger.
-
(C1): Located between A2 and A3
-
(C2): Between A3 and A4
-
(C3): Lies between A4 and A5.
Oblique pulley – 1 associated with the thumb.
Any injury within the following regions (ex: cut)
Hand Zones
5 flexor tendon zones (injury)
Zone I: Extends from the fingertip to the mid-portion of the middle phalanx. Point of FDS insertion
Note: FDS attaches to the middle phalanx whereas FDP reaches till the distal phalanx, so if there is tendon cut in zone I it is definitely FDP as it reaches the distal phalanx
Zone II: From the mid-portion of the middle phalanx to the distal palmar crease. Called: “No man’s land”
Zone II is the most difficult zone to work with (worst prognosis) because it has FDS, FDP, lumbricals, palmar interossei, blood vessels and nerves
Zone III: From the distal palmar crease to the distal border of the transverse carpal ligament
Zone IV: Overlies the transverse carpal ligament
Zone V: From the wrist crease to the level of the musculo-tendinous junction of the flexor tendons

Zone I: DIP
Zone II: middle phalanx
(mallet finger)
A lesion of the terminal extensor tendon (zone 1 or 2) can be open or closed and can have an associated fracture, tear, or avulsion of the terminal extensor tendon
Symptoms: Unable to extend distal phalanx/ Edema may be present.
Zone III: PIP joint
Zone IV: proximal phalanx
(Boutonniere deformity)
Occurs after a rupture in the central slip Zones 3
or 4Forces DIP joint into extension and PIP into
flexion,it is not immediately developed with
closed injuries. It will take about 2-3 weeks after
the injury.
Symptoms: Inability to extend PIP & flex the DIP
joints/ Tenderness at the site of injury/ Edema
(swelling).
It can result in a stiff finger if not treated
Zone V: MCP joint
Zone VI: metacarpals
Zone VII: wrist (carpus and extensor retinaculum)
Zone VIII: distal third of the forearm
Swan neck deformity: (opposite of Boutonniere deformity) it is a tear of PIP volar plate or finger trauma
Resulting in flexed MCP, extended PIP, and flexed DIP
Symptoms: Pain, swelling, PIP hyperextension = Indication of volar plate tear
injury in which a body structure is torn off by either trauma or surgery in this case the tendon can pull the edge of the bone of the distal phalanx

Proximal Humerus Fracture: Most common type of humerus fractures, may involve articular surface, greater/lesser tuberosity, or surgical neck. Can be one-part, two-part fractures, three or four-part fractures
Frozen Shoulder: Called adhesive capsulitis, or frozen shoulder
primary - idiopathic in nature, could be from inflammation, biochemical or immune imbalance.
secondary - precipitating from an event such as trauma or surgery
There are three stages for this injury: freezing, frozen, thawing.
-
Freezing phase: experiencing shoulder pain in sleep and ADLs. In the following 2 to 9 months, the pain decreases and is felt at the end of motion.
-
Frozen phase: may last up to a year, pathological movement pattern develops, pain is felt while stretching at the end of motion.
-
Thawing phase: gradual return of motion, lasts an average of 24 months, could take between18 months to 3 years to complete all phases.
Glenohumeral Instability: GH instability is opposite of frozen shoulder. instability exists when laxity leads to pain with loss of power
Laxity: The amount a joint or ligament deviates from its initial position when a force is applied to it
Elbow stiffness is the most common complication. The more severe the trauma, and the longer the period of immobilization, the more likely the loss of motion and stiffness to develop. Flexion contracture is the most common type.
Radial head fractures: most common, results from falling on outstretched hand w/ forearm pronated.
Olecranon fractures: results from falling onto or due to direct blow to elbow.
Distal humeral fractures: relatively uncommon, usually associated with RTAs or sports injuries.
Fracture can be either simple (closed) or compound (open)
Fracture Terminology
-
Incomplete (Greenstick)
-
Complete
-
Comminuted
Can be
-
Oblique
-
Transverse
-
Spiral
Located
-
Base
-
Mid-shaft / Body
-
Neck
Signs and symptoms:
-
Pain
-
Edema
-
Bruising
-
A limb or joint is visibly out of place
-
Limitation of movement
-
Numbness & tingling
-
Paleness of the injured area
Distal Radius fracture
-
Colles’ Fracture (outward): after a fall on an outstretched hand (also called Silver fork deformity)
•Distal displacement of the distal fragment
-
Smith’s Fracture (inward)
-
Palmar displacement of the distal fragment
-
Reverse Colles
-
Second most common distal radius fracture
-
Frequently unstable
-
Typically require internal fixation
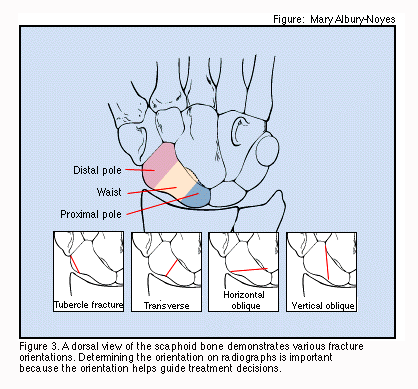
Scaphoid fracture is the most common carpal bone fracture
-
Has a proximal pole, a distal pole, and a waist.
-
Retrograde blood supply
-
The blood supply enters at the distal pole
-
Poor blood supply to proximal third
Caused by a fall on an outstretched hand
Signs and symptoms:
-
Wrist aches
-
Pain over snuff box
-
Painful handshake or with overpressure
-
ROM is restricted
-
Particularly wrist extension
-
Grip strength is reduced by more than 50%
Joint stiffness is caused by a limited range of motion of a joint, not by weakness or reluctance to move the joint due to pain. Some people with stiffness can move the joint through its full range of motion, but this movement can require force.
Limitations can include tendon and skin excursions, edema, tenosynovitis, adhesions... etc.
An adhesion is a pathological band restricting the normal movement between two adjacent tissues.Can result from inflammatory response or a traumatic incident, or surgery.
Tissue tightness is also referred to as shortening in the muscle, tendon, or ligament of a specific joint.
A local or generalized condition in which the body tissues contain an excessive amount of tissue fluid. Edema is a symptom, not a disease!
Characterized by an increase in the interstitial fluid in intercellular tissue spaces.
Edema becomes apparent when the interstitial fluid is at least 30% above normal
Localized edema
Causes:
-
Increased blood vessel wall permeability like Inflammation.
-
Increased capillary pressure like Venous obstruction or heart failure
-
Lymphatic obstruction
-
Disturbances in renal functioning
-
Chemical substances such as bacterial, toxins, venoms, histamine, ...etc.
-
It may be the result of trauma or infection
-
Tends to be limited to one area of the body
Types of Edema
-
Pitting edema: When pressing on the skin, it causes an indentation that persists for some time. ◦ Causes: Systemic diseases, pregnancy, heart failure, Or local conditions such as varicose veins, insect bites, and dermatitis.
-
Non-pitting Edema: Observed when the indentation does not persist. Associated with conditions such as lymphedema, lipedema, and myxoedema.
High Radial Nerve Lesion causes:
-
Wrists drop
-
Inability to extend MCP joints
-
Diminished thumb extension and abduction (EPL, EPB & APL paralysis)
-
Weakened power grip
-
Weakened supination
-
Loss of sensation of lateral 2/3 of dorsum of hand and lateral 3 digits.
Posterior Interosseous Nerve Lesion causes:
-
The posterior interosseous nerve is a motor branch of the radial nerve
-
Same as radial nerve lesion, except:
-
No sensory loss
-
Wrist extension is present, but weakened
-
ECRL is not paralyzed
High Median Nerve Lesion causes:
-
Same as low median nerve lesion (below), in addition to:
-
Loss of pronation
-
Weakened wrist flexion
-
FCU is intact
-
Weakened finger flexion
-
Paralysis of all FDS
-
Paralysis of FDP of index & middle digits
-
FDP of ring & little digits is intact
Low Median Nerve Lesion causes:
-
Sensory loss of median nerve distribution
-
Loss of thumb coordination
-
Decreased grip/pinch strength
-
Loss of APB & OP muscles
-
Ape hand deformity:
-
Loss of lateral two lumbricals
-
Hyperextension of lateral 2 MCPs
-
Cannot fully extend index and middle fingers
-
Cannot move the thumb outside of the plane of the palm
-
Inability to oppose the thumb
-
Limited abduction of the thumb
-
-
High Ulnar Nerve Lesions
-
Same as low ulnar n. lesion (below), in addition to:
-
Weakened wrist flexion (paralysis of FCU).
-
Weakened finger flexion(paralysis of FDP of ring &little digits).
-
Low Ulnar Nerve Lesions
-
Sensory loss of ulnar nerve distribution
-
Loss of fingers adduction and abduction
-
Weakened thumb adduction
-
Claw hand deformity:
-
Loss of ulnar n. for the two lumbricals (ring and little fingers)
-
Causes hyperextension at MCPs
-
Cannot fully extend ring and little fingers
-
-
A burn is an injury to the skin primarily caused by heat, radiation, electricity, friction, or contact with chemicals (WHO).
1. Scald (Hot liquid) Water, steam, cooking oil, etc.
2. Open flame
3. Hot surface contact E.g, iron
4. Electrical and chemical injuries
5-10% of all burns
-
Radiation:
-
X-rays, UV lights, etc.
-
-
Friction:
-
Mainly car accidents
-
Radiation:
-
X-rays, UV lights, etc.
-
Friction:
-
Mainly car accidents
-
Burns can be classified according to:
1. Depth (Degree)
2. Extent (%)
3. Severity
1. Depth
1. Superficial: affects only the epidermis and heals within days
2. Superficial Partial Thickness: Epidermis and dermis, excluding all dermal appendages which include hair follicles, sweat glands, and sensory receptors.
3. Deep Partial Thickness: Epidermis and most of dermis (minimal dermal appendages)
4. Full Thickness: Epidermis and all of dermis
2.Extent
Burn injuries are also classified in terms of the percentage of the skin surface injured (TBSA)
Rule of 9’s: A relatively simple, but not totally accurate, method for determining the extent of injury
-
Head = 9%, (18% for the child)
-
Arms = 9%,
-
Legs = 18% (each) (13.5% for the child)
-
Anterior trunk = 18%
-
Back = 18%
-
Perineum/Genitalia = 1%

3. Severity Grading of Burn

-
First-degree (superficial) burns. only affect the outer layer of skin, the epidermis. The burn site is red, painful, dry, and with no blisters. Painful ++, and No scarring/ can be treated with conservative therapy
-
Second-degree (partial thickness) burns. affect the epidermis and part of the lower layer of skin, the dermis. The burn site looks red, blistered, and may be swollen and painful. Painful+++. No scarring, there might be discoloration/ can be treated with conservative therapy
-
Third-degree (full thickness) burns. destroy the epidermis and dermis. They may go into the innermost layer of skin, the subcutaneous tissue. The burn site may look white/blackened and charred/wet. Painful +. Scarring/ needs a surgery
-
Fourth-degree burns. it goes through both layers of the skin and underlying tissue as well as deeper tissue, possibly involving fat, nerve, muscle, and bone. There is no feeling in the area since the nerve endings are destroyed. Leathery, dry, waxy, charred. Painless. Scarring/ need surgery.
Complications: Scar contracture
-
Hypertrophic scar: Confined to wound margin because of the production of excessive amount of collagen, which produces a raised scar, reaches a certain size, and subsequently stabilizes or regresses
-
Keloid scar: Grows beyond the boundary of the original site of a skin injury
Heberden’s nodes DIP:
Hard bony lumps in the joints of the DIP. These nodes are osteoarthritis that result from the breakdown of the cartilage due to slow wear and tear over time or from joint injury. This will make the smooth cushioning in the joints rough which causes pain, stiffness, and inflammation.
The symptoms are:
-
Stiffness
-
Pain
-
Swelling.
-
Weakness.
-
Crepitus. Means grinding, cracking, or clicking that happens when moving hands.
Bouchard’s nodes PIP:
is the same as Heberden’s but the only difference is that Bouchard’s is on the PIP and is more common.
It is a hand deformity that usually takes years to develop. It affects a layer of tissue that lies under the skin of the palm and gradually creates a thick cord that can pull one or more fingers into a bent position. This prevents them from being able to extend completely. It commonly affects the two fingers that are on the ulnar side away from the thumb and is usually painless. This deformity will have a huge impact on decreasing the strength and the ROM of the wrist if its not treated
Grip Strength
-
The client will be in a sitting position, the shoulder adducted, elbow flexed to 90 degrees, and forearm and wrist in neutral.
-
the dynamometer will be placed to the client’s hand by the therapist to suppor the base of the dynamometer,
-
the client will be instructed to squeeze as hard as possible. without rapid jerking motion and the force is smoothly applied to the dynamometer, Allowing the wrist to extend during the grip.
-
The test is Three trials. You have to alternate between hands in each trial, for example, start with right and then go to the left and then repeat the trail. After that compare the results.
Note: Before performing strength testing, check any contraindication or precaution. precaution: any tendon that is in the process of healing
contraindications: any dislocation or fracture as they are
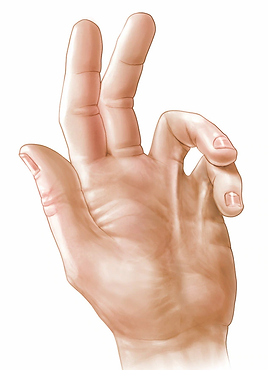
Pinch Grip Test: same steps for the grip strength
-
Lateral pinch (key pinch): the Pinchmeter is placed between the radial side of index finger and thumb, then the client is instructed to apply force like he is holding a key
-
Three-point pinch tripod: the Pinchmeter is placed between the pulp of the thumb, index, and middle finger. the client is instructed to pinch as hard as possible.
-
Two-point pinch (tip to tip pinch): the Pinchmeter is placed between the tip of the thumb and tip of the index finger, then the client is instructed to pinch as hard as possible.
Phalen test for (CTD) :
To get a positive result in this test the patient has to hold the wrists together in a flexed position against each other in 90 degrees facing the dorsal side for a whole minute. pain, tingling, and numbness will be felt in fingers because of the median nerve distribution at the level of the carpal tunnel.

Tinel sign:
this test is positive when tingling or "pins and needles" are presented when lightly tapping (percussing) over the nerve. Can be on median nerve and Ulnar never for CTD
Froment’s sign:
To get a positive in the test when the muscles of the adductor pollicus of the thumb is weak when doing the pinch grip strength also when trying to do the lateral pinch the thumb IP is flexed due the damage to the ulnar nerve that innervate this muscle. It tests the strength of the adductor pollicus of the thumb,)
Wartenberg’s sign (5th finger is abducted):
It is a sign of ulnar nerve weakness that innervates the intrinsic muscle (the abductor digiti minimi, Opponens Digiti Minimi and Flexor Digiti minmi also the ulnar nerve innervates the dorsal and palmar interosseous muscle.
Finkelstain’s test:
A test used to diagnose de Quervain's tenosynovitis in people who have wrist pain. To get a positive sign in this test pain should be present in the first dorsal compartment when doing thumb adduction in the palm, with Ulnar deviation of the wrist.


Volumeter:
Used to test the size of edema in the hand. The steps of this test are: first placing the volumeter on a stable flat surface. The second step is to fill volumeter until it overflows. Then the 3rd step is the client slowly lowers the hand into volumeter until dowel rod that is in the base of the volumeter rest in the webspace between the middle & ring finger. Make sure that the hand is not pressing on the rod but lightly touching its. The final step the client maintains in this position position until water no longer is displaced and take the readings.
Figure of 8:
Sometimes some cases cannot be put in the water as they have some affectes figure of 8 is another way to measure the size of the edema. The steps of this test are starting at the Pisiform bone hold the tape at it and move the tape measure diagonally across the dorsal aspect of the hand, moving toward the 2nd MCP joint line Bring the tape measure across the ventral surface of the MCP joints and moving toward the 5th MCP joint; The tape measure is wrapped diagonally across the dorsum of the hand back to the starting point. To see if you are doing the steps correctly a figure of the number 8 will be shown at the dorsal aspect of the hand.
Total Active Motion (TAM):
The Sum of degrees of active MCP, PIP & DIP (ROM) flexion TAM norm = 260-280 depend on the normal ROM degrees or you can use the contralateral finger as the normal to compare The TAM of the injured finger is divided by the norm (either contralateral total or 260-280°). The result is the percentage of normal.

ROM :
Is a teste reading are taking comparing with the other normal (uninjured hand or from the normal range reading
The reading is taken through the gonio meter depending on the join the axis is position on the join and the moveable arm is going with the movement of the joint
DASH:
The Disabilities of the Arm, Shoulder and Hand (DASH): is a 30-item questionnaire that focus on the ability of the patient to perform certain upper extremity activities. it is a self-report questionnaire that patients can rate difficulty and interference with daily life activities on scale of 1 to 5. Scoring will be the sum
of the total results over the number of the items. Note that dash cannot be completed if more than 3 items are missing.
Sollerman Hand Function Test
Is a test to measure the ability and the quality of the hand functions when preforming the activities of the daily living, there are 8 main hand grips in ADLs Pulp pinch, lateral pinch, tripod pinch, five finger pinch, diagonal roller grip, transfer volar group, Spherical volar grip, extension group

Symptom Severity Scale:
It is a questionnaire that it used mostly for carpal tunnel syndrome measure the severity of the symptoms grading from 0 to 3
-
0 for No problems
-
1 for Mild: It comes and goes.
-
2 for Moderate: You usually have or feel it.
-
3 for Severe: It seriously affects your daily life
Patient Specific Functional Scale
It is self-report outcome measure of function for levels of independence of the patients.
The patient identifies five important activities that they are unable or have difficulty to perform and then they have to rate it (on an 11-point scale) the current level of difficulty associated with each activity. After the intervention, the patient is required to rate the activities again and they can also name new activity that have difficulty to perform within the time that was passed. "zero" represents “unable to perform” and "10" represents “able to perform at prior level”. Patients select a value that best describes their current level of ability on each activity assessed.
Two-point discrimination
This test is used to evaluate the ability to discriminate the two points of touch. It is assessed by using a small tool with prongs at a fixed spacing from 2mm to 15mm. Should only be used when the skin has a sensory return of light touch. And this will reflect how finely innervated an area of skin. The therapist will apply the test on the patient area being tested while the patient's is vision occluded. Starting on a 5mm distance between the two points the therapist Randomly place either 1 or 2 points parallel to the long axis of the finger and then the patient is asked whether 1 or 2 points has been felt. If the responses are inaccurate then the distance between the two endpoints is increased by increments of either 1,2 or 5mm
Monofilament:
This test is used to assess the threshold perception of light touch to deep pressure. This test should be done in a quiet area with vision occluded and applying it from distal to proximal and from small to large monofilaments. The patient's hand should be supported to avoid moving the finger, especially when using the larger filaments. The therapist applies the pressure the monofilament should be at 90 degrees. Then the patient is Instructed to respond when they feel the pressure, Press the filament at a 90-degree angle for 1.5 seconds against the skin until it bows and then removes.
-
RICE :
-
Rest: protect the injured area and rest it. avoid any activity that can affect the injury and cause pain or soreness.
-
Ice: Cold will reduce pain and swelling and if swelling is gone, apply heat to the area that hurts (hot and cold pack techniques):
-
slowing the body’s metabolism and its demand for oxygen. It Slows or stops bleeding and relieves pain
-
The Hot Pack: Brings more blood to the area where it is applied. Reduces joint stiffness and muscle spasm, which makes it useful when muscles are tight. And Relaxes tight muscles causing tissues to relax. In the session hot pack usually be applied at the beginning of the session to make the scar message and breaking the adhesion from surgery much easier
-
-
Compression: Compression the injured area with an elastic bandage this will help to decrease swelling. However, this should be applied in a weighted balance as to much compression (tightly) will cause more swelling below the affected area
-
Coban spiral warp
-
Elastic gloves
-
-
Elevation raising the injured area above the level of the heart. Will reduces pain, throbbing, and swelling.
-
-
Light retrograde massage
Is to reduce swelling in the hand. The massage is done manually by applying moisturizer and moving fluid from the tips of the fingers back toward the heart (from distal to proximal).
-
Elevate the hand above the elbow and heart level
-
Administer for almost 10 min.
-
Use a moisturizer to reduce friction
-
Keep the wrist in a neutral position
-
Massage from the tips of the fingers down toward the elbow, both the front and back of the hand.
-
Scar massage
Many of the patients who need hand therapy have had a surgery. Having a surgery in the hand without starting rehabilitation immediately leads to scar formation in the area of the surgery, resulting in adhesion. Although scar formation is important for healing, too much scar irritates the healing process.
One of the effective techniques used by occupational therapists to manage this problem is massaging the scar. It is an intervention used to soften and flatten the hard scar tissue, because it may stick to the underlying muscles, tendons, blood vessels, nerves, and bones. Scars may feel sensitive, tingle or pain when touched so regular massage can help to control this.
The method of scar messaging is:
-
apply a non-perfumed moisturizing cream on the area of the scar.
-
Place the pad of your thumb on the scar and massage using a slow, circular motion so that the skin moves on the underlying scar tissue.
-
Repeat this process across the entire scar using firm pressure without causing any damage to the skin.
-
Keep doing this for at least 10 minutes, or until you feel the adhesion getting softer.
-
Sensory Management (Resensitization)
Occupational therapy deals with sensory problems because there is a close connection between motor & sensory systems, especially in the hand. Sensory loss in hand causes impaired fine motor coordination & manipulative ability leading to weak grip because of decreased degree of force. Sensory impairment causes a risk of injury. Resulting inappropriate Fine touch & proprioception, Temperature sensation, and inappropriate Pain sensibility. Using tough textures from the sensory the therapist provides cues to observe the affected limb visually to reconnect the neural pathways between the brain and the limb to improve sensation
-
Vibration Machine
When there is a patient with a hand tumor, tendon rupture, or any hand injury that causes pain, the therapist is most likely to use the vibration machine. This technique is used with patients who have hypersensitivity due to desensitization by enhancing circulation. From the therapists’ experiences, the vibrator also helps in scar management to facilitate healing. The way of using the machine is very easy.
-
Set the vibration speed to be moderate and tolerable for the patient.
-
Apply the vibrator on the area of pain and scar with moving it in circular motion.
-
Keep moving it on the whole area for 10 minutes.
In some cases, the vibration machine cannot be used because it may cause other complications.
-
People who have a pacemaker.
Overall, this technique is very effective and lead to fast improvements. Another advantage of this technique is that the patient can buy a machine and use at home as a home program, which helps is faster recovery.
-
Tendon gliding
An injury to the hand or finger can result in increased swelling, scar formation and adhesion, which limits how the tendon glides, and ultimately affects joint range of motion, loss of strength, decreased coordination and reduced ability to use the hand. In this case the patient needs to perform tendon gliding exercise as a treatment.
The tendons that are used:
-
Flexor Digitorum superfecialis
-
Flexor Digitorum profundus
The occupational therapist can go through tendon gliding exercises to help move the tendons individually as well as together to give the best movement possible. It also has the benefit in reducing swelling.
The tendon gliding exercises can be used with different conditions:
-
Arthritis
-
De quervains
-
Trigger finger
-
Flexor tendon repair
How to do the exercise?
-
Start with the fingers straight.
-
Flex the DIP and PIP joints, whilst keeping the MCP joints extended.
-
Flex the MCP joints with extending the IPs.
-
Touch the palm keeping the DIP extended
-
Make a full fest.
-
Strengthening exercise throw tools and their colors
Some exercise is giving depending on the case, wrist extension, finger flexion and there are some tools that are used with various of color and their strength This is general however take note of your case and make sure to give it the right color
-
beige 0-2 weeks
-
yellow 2-4 weeks
-
red 4-6 weeks
-
green 6-8 weeks
-
blue 8-10 weeks
-
black 10-12 weeks
Flexor tendon treatment: (guideline)
-
Precautions: No active flexion, no passive extension
-
Early controlled mobilization (Kleinert)
-
AKA passive flexion protocol
-
Early active mobilization
-
Immobilization
Extensor tendon treatment:
-
Precautions: No active extension, no passive flexion
-
Immobilization
-
Early passive mobilization
-
Splint:
-
mallet finger
-
Swan neck deformity splint.
-
Boutonniere deformity splint
-
Ergon techniques (need special studies/ certification)
It is a special designed stainless-steel equipment-tools used as an innovative treatment method for mobilizing soft tissues of the body it
-
detect and release – loosen scar tissues, adhesions, and fascial stiffness,
-
increase localized perfusion.
-
decrease muscle tone and muscular pain.
-
Reducing edema and hematoma
-
Improve the blood and lymphatic circulation.
-
increase of the range of motion in joints.
-
increase the speed of the healing by increasing cellular activity.
There are many patients with different hand injuries that need a specific type of splint for different reasons. Hand splinting is very helpful and can be used for many advantages:
-
Supporting damaged joints to increase your strength
-
Positioning the hand appropriately
-
Reducing stress on painful or damaged joints
-
Reducing pain
-
Providing a cue about how to use the joint more carefully and a cue to others to be careful around the hand
-
Immobilize the joint.
-
Increase and maintain ROM
-
Prevent contractures and stiffness
Low Temperature Thermoplastics is required to Softens with low heat at 60o – 75o C (140o - 170o F) Warm water allows consistent and overall coverage and the Heat gun is used for spot heating or dry heat
Categories of Splints
-
Static splints: A splint that is molded to maintain the tissue in one position and does not have moveable parts, it is used to relive pain, Position and maintain joint alignment, Prevent adaptive shortening of soft tissue, Correct soft tissue contractures, and Immobilize a joint or limb following trauma
-
Dynamic splints: A splint that applies force and movement to a joint(s). Used to assist weakened muscles, Substitute for lost muscle function, and minimize adhesions formation. There are three parts:
-
splint base
-
dynamic traction force
-
outrigger
-
-
Static progressive splints (Serial static splints): Similar to dynamic splints, but missing the movable components, applies low load to joint while maintaining the tissue at its maximum length. Worn for extended periods of time so that the tissue adapts “grow” to its new length May be used to Increase range of motion, correct soft tissue contractures, and maintain improvement obtained through other forms of treatment, such as passive stretching.
Properties of Splints
-
Rigidity: strength of the material, High rigidity does not bend easily are preferably to use for large joints
-
Memory: ability to return to its original shape and size when re-heated, Material with excellent memory usually takes longer to harden
-
Drape-ability (Conformability): Ability of material shape around and mold over contours of an extremity
-
Bonding & Coating: ability to stick to itself or to other material when heated
-
Working Time: The amount of time it takes the material to cool, the less working time the more suitable for children.
-
Thickness: Thinner materials are better for small joints and children. Thinner material cools off faster
-
Perforation: Allows better ventilation of the skin, Ideal for warm or humid climate
-
Splint Accessories
-
-
Sticky-backed Velcro: Bonds best when heated (dry heat), Rounded corners prevent “catching”
-
Padding: Bonds best when heated (dry heat), Changes fit of splint (smaller, tighter)
-
There are different types of hand splints for different cases: Some examples:
-
Thumb Spica splint
-
Cock-up wrist splint
-
C-bar static splint
-
Swan neck deformity splint.
-
Boutonniere deformity splint
-
Trigger finger splint
-
CMC static splint
-
Static Progressive Splint - 3-Point Design
-
Dynamic splint Kleinert and Modified Kleinert
The splints should be done with considering some principles:
-
No demarcations
-
A conforming fit reduce unequal pressure
-
Avoid pressure over bony prominences
-
Use padding over bony prominence before splinting.
-
Smoothed, rolled, or rounded edges reduce pressure sores
Round corners to avoid sharp points.
click on the file for picture
Power Web
-
It is a color-coded tool in which the resistance increases according to the color (Beige, Yellow, Red, Greed, Blue, and Black)
-
It is used for developing strength of hand muscles, and range of motion of the finger joints (IPs)
…………………………………………………………………………………………………………
Cando Digi Flex
-
Color coded resistance tool (Yellow, Red, Green, Blue, and Black)
-
This tool is used for improving finger strength, and coordination.
-
It is used for many cases: -carpal tunnel syndrome -arthritis -stroke -Fractures -Flexor tendon repair -nerve lacerations
…………………………………………………………………………………………………………
Theraputty
-
The resistance is increased according to the color.
-
It is used in finger, hand, and wrist resistive exercises.
-
Some exercises are: - Full grip -Finger extension -Pinch gripping
-
It helps in improving fine motor skills, gripping strength and dexterity.
………………………………………………………………………………………………………
Finger Ladder
-
Wall-mounted shoulder rehabilitation equipment.
-
The ladder is divided into 36 steps, separated by 1.25" intervals
-
Use in standing or seated positions
-
Evaluate range of motion.
-
It helps enhance overhead reach and improve ROM and flexibility of shoulder, elbow, wrist, and fingers.
-
Can be graded up by wearing a weighted cuff.
………………………………………………………………………………………………………
Massage Star
-
This tool is used for scar messaging.
-
After a hand surgery for any injury, most patients develop a scar tissue that needs management.
……………………………………………………………………………………………………………
Weights (Dumbbells)
-
Used for strengthening
-
They can be used after 8-12 weeks during the treatment of flexor tendon repair
-
Active assistance: The hand of the patient can be wrapped with the weight by a bandage.
………………………………………………………………………………………………………
Pronation and supination wheel
-
This tool is used for patients having problems is doing pronation and supination because of: - Stiffness - Muscle weakness –Fracture
-
It helps in strengthening wrist muscles and improving the pronation and supination ROM.
-
It can be used to observe the improvement of ROM without measuring.
………………………………………………………………………………………………………
Resistive Pinch exerciser
-
It is a color-coded tool with increasing resistance ( Yellow, Red, Green, Blue, Black)
-
It is used to improve the strength of finger pinch: - Lateral pinch -tip to tip - Tripod
-
It helps to improve fine motor skills and fingers coordination.
-
Vertical and horizontal rods are used to improve wrist ROM.
………………………………………………………………………………………………………
Digi-Extend finger exerciser
-
This tool has changeable graded resistance rubber bands.
-
Used to strengthen the intrinsic and extrinsic muscle groups to maximize extensor tendon gliding,
-
Helps to improve IPs ROM of Extension.
-
It can also be used for finger adduction, abduction, blocking, and flexion exercises.
……………………………………………………………………………………………………………
Shoulder Arch:
-
This tool is used to improve the ROM of shoulder flexion and horizontal adduction and abduction.
-
It is also used in improving crossing the midline, pinch strengthening, and improving hand-eye coordination.
-
Can be graded up by adding more pipes.
………………………………………………………………………………………………………
Shoulder Exercise ladder
-
It is used to improve the ROM of the shoulder flexion and extension.
-
Used to improve the shoulder muscles strength.
-
Can be graded up by adding weighted cuff to the dowel rod.
………………………………………………………………………………………………………
Stacking cones
-
It is used for shoulder ROM of flexion, extension, horizontal adduction, and abduction.
-
Used for hand grip strength and eye-hand coordination.
-
Can be graded up by wearing wrist weighted cuff.
………………………………………………………………………………………………………
Sensory box
-
The boxes are filled with different materials numbered according to textures (Rough, Soft)
-
Textures are used for desensitization and resensitization interventions.
-
Small objects with different textures are hidden in the box and the patient is asked to put his hand inside and find them.
……………………………………………………………………………………………………………
Zen Hand exerciser
-
This is a resistive exercising tool that is color coded.
-
It is used to strengthen finger extension.
-
It can be used for patients with: -arthritis -RSI -carpal tunnel -tennis elbow -stroke -MS
……………………………………………………………………………………………………………
Rough ball and sponge
-
It is used for sensory re-education
-
Patients with sensory loss, because of nerve injury, stroke, or TBI, use these objects to improve sensation.
-
The sponge can also be used for desensitization when the patient feels pain.
…………………………………………………………………………………………………….
Pegboard
-
It is used to improve coordination during hand and finger.
-
help increase proprioception, strength, and general motor skill
click on the file for pictures
Physiopedia:About - Physiopedia (physio-pedia.com)
Trigger finger - Symptoms and causes - Mayo Clinic
Hand & Forearm Compartment Syndrome - Trauma - Orthobullets
thank you for Dr.Mohammed Nader for the notes and education