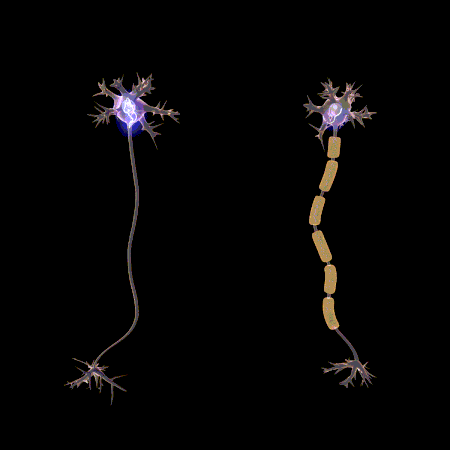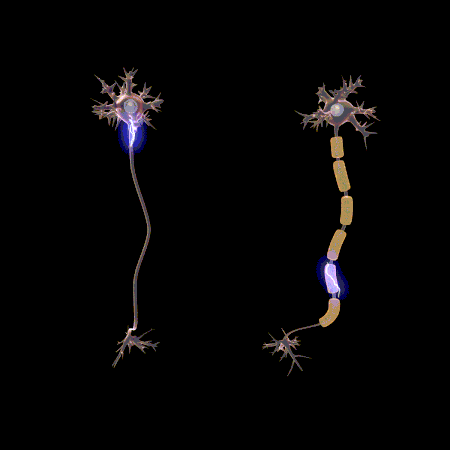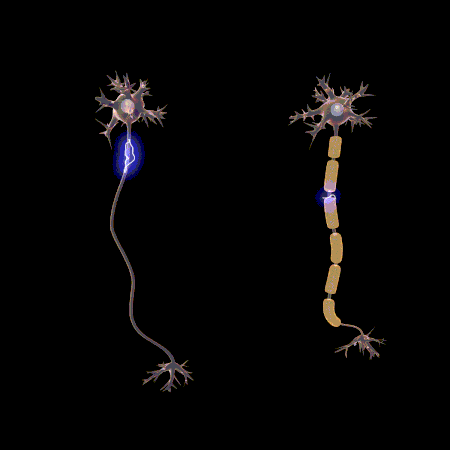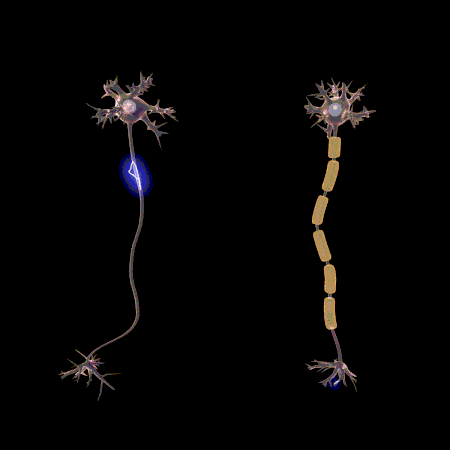
Neurology
-
Try to make you session meaningful and purposeful
-
Try to incorporate your client's priorities and concerns
-
To to achieve the best possible outcomes for your client, try to work closely with members of an interdisciplinary team of physicians, physical therapists, speech therapists
Definition:
It is a disease of cerebral vasculature causing a failure to supply oxygen to the brain.
Impairments following stroke can affect:
-
Perception
-
Sensory
-
Cognition
-
Motor Control
-
Upper Limb Function
-
Shoulder Subluxation
-
Pain
-
Voluntary control
-
Occupational Performance Areas
Internal capsule
Basal Ganglia
Stroke classifications described in table1:

Table 1
[1] The space that exists between the arachnoid and the pia mater.
Table 2 describes the function of the external structures of the brain:

Table 2
Cranial nerves: (table 4)

Table 4
2- The artery that is involved:
-
Internal carotid artery
-
Middle cerebral artery
-
Anterior cerebral artery
-
Posterior cerebral artery
-
Cerebellar artery
-
Vertebra-Basilar artery
Table 3 describes the impairments associated with each artery:


Table 3
[4] Defective vision or blindness right or left halves of visual fields of both eyes.
[5} Broca’s aphasia: speech production / Wernicke’s aphasia: language comprehension
[6] Ideational apraxia: inability to carry out tasks in the proper order/ ideomotor apraxia: individual is able to perform task automatically but unable to carry the movement on command
[7] Fail to report, respond or orient to meaningful stimuli presented on the affected side
[8] Fail to distinguish an object from background
[9] Defects confined mostly to about one fourth of an eye's visual space
[10] The inability to orient in the surrounding, inability to find the way in a large environment
[11] The ability to identify or sort objects, shapes, symbols, letters, and/or words, despite differences in size or position.
[12] Inability to recognize and identify objects, persons, or sounds correctly
The Symptoms depend on:
1- The part of the brain that loses blood supply:
-
Thalamus:
-
Anterolateral: Visual neglect
-
Lateral: sensory symptoms
-
Bilateral: memory deficits
-
Posterior: alert/ conscious
-
-
Internal capsule: Pure motor dysfunction
-
Basal ganglia: dysarthria*and lack of initiative
-
Cerebellum: Ataxia**
*A motor speech disorder in which the muscles that are used to produce speech are damaged, paralyzed, or weakened.
**Lack of voluntary coordination causing gait abnormality.
Definition:
TBI is an insult to the brain caused by an external physical force with resultant loss of consciousness.
It can be either closed or open brain injury:
-
Closed brain injury:
-
No penetration to the skull
-
Resulting from falls, motor vehicle crashes
-
Focal damage* and diffuse damage to axons
-
Effects tend to be broad (diffuse)
-
-
Open brain injury:
-
Penetration to the skull
-
Focal damage and some diffuse damage
-
Changes after TBI:
-
Loss of consciousness/ coma
-
Post-Traumatic Amnesia (PTA): s a state of confusion that occurs immediately following a traumatic brain injury (TBI) in which the injured person is disoriented and unable to remember events that occur after the injury.
-
Ataxia: Impairment of the cerebellum or tracts from it along with impaired proprioception.
-
Incoordination
-
Impaired standing
-
It occurs in the entire body
-
Ranges from mild to severe
-
-
Tone Abnormality: Hypotonicity to Hypertonicity during recovery at higher cognitive level/ Rigidity during the comatose stage.
-
Limitations of Joint ROM: Before initiating intervention, OT need to determine with the physician cause of decreased ROM.
-
Cognitive deficits which include:
-
Attention and concentration
-
Processing of information
-
Memory
-
Executive functions: plan, organize, set goals
-
Abstract thinking: ability to hold and manipulate a concept in one’s mind
-
Impaired initiation and termination of activities
-
Speech and communication
-
-
Psychosocial Skills: Loneliness/ decreased in relationships: so the Family is a primary source of social and leisure activity for many persons with TBI.
*Widespread cerebral injury
**Localized injury in the brain occurring immediately after the injury and easily visualized by CT or MRI
Vertebral column consists of 33 vertebrae:
-
7 cervical
-
12 thoracic
-
5 lumbar
-
5 fused sacral
-
4 fused coccygeal
Spinal cord:
It is a long, thin, tubular structure made up of nervous tissue which extends from medulla oblongata and end in L1/L2
Spinal nerves:
The spinal nerves are relatively large nerves that are formed by the merging of a sensory nerve root and a motor nerve root. These nerve roots emerge directly from the spinal cord sensory nerve roots from the back of the spinal cord and the motor nerve roots from the front of the spinal cord. As they join, they form the spinal nerves on the sides of the spinal cord.
There are 31 pairs of spinal nerves including:
-
Eight cervical spinal nerves on each side of the spine called C1 through C8
-
Twelve thoracic spinal nerves in each side of the body called T1 through T12
-
Five lumbar spinal nerves on each side called L1 through L5
-
Five sacral spinal nerves in each side called S1 through S5
-
One coccygeal nerve on each side, Co1
Dermatomes: (check picture 2 and 3)
-
Area of skin innervated by sensory axons within a particular segmental nerve root.
-
Important to determine the level of injury.
-
Useful in assessing Improvement and deterioration.
Myotomes: (check picture 2 and 3) + Table5
-
Segmental nerve root innervation a muscle.
-
Important in determining level of injury.


Picture 2
Picture 3
Picture 1


Table 5
Spinal cord injury (SCI): insult to spinal cord resulting in a change in the normal function either temporary or permanent:
-
Motor
-
Sensory
-
Autonomic
Complications following spinal cord injury:
-
Pressure sores
-
Spasticity
-
Orthostatic Hypotension
-
Autonomic Dysreflexia
-
Heterotopic ossification
-
Osteoporosis
Classifications of SCI:
-
Skeletal and neurologic level: the regions of SC which they occur (cervical, thoracic, and lumbar) and the numerical order of the neurological segments.
-
Ex: C6 refers to the 6th neurological segment of the cervical region of the SC as the last fully intact neurological segment.
-
-
Completeness (degree of injury):
-
Complete injury: Absence of sensory and motor function in the lowest sacral segments (S4-S5) > no sacral sparing
-
Incomplete injury: preservation of any sensory and/ or motor function below the neurological level > presence of sacral sparing. (check table 6)
-
Classifications of incomplete SCI and associated impairments: (Table 6)

Table 6
Level of injury in spinal cord injury and extent of paralysis described in table 7:

Table 7
Amylotrophic lateral sclerosis (ALS): It’s a group of progressive, degenerative neuromuscular diseases, also known as motor neuron disease.
-
The neurologic process involves destruction of motor neurons within the spinal cord, brainstem, and motor cortex.
-
Affected individual exhibits combination of both Upper motor neuron and Lower motor neuron deficits, including:
-
Abnormal fatigue
-
Decreased strength
-
Speech deficits (slurred speech)
-
Spasticity, muscle cramps
-
However, cognition, bowel and bladder, sensory, eye function are not affected early.
-
Functional stages of ALS:
The early stage:
-
Patient experiences generalized fatigue and specific localized weakness to one side of the body, one limb or upper or lower trunk.
-
The ADLs are specifically impaired.
The disability stage:
-
ADLs and function are very limited, all extremities and trunk show significant signs of limitation.
-
Caregiver roles are significant.
The end stage:
-
Patient becomes nearly fully dependent on caregiver for most if not all ADLs.
-
Very minimal to no function in all extremities.
-
The patient positioning is limited to the bed or to the wheelchair (preferably powered wheelchair).
Huntington's disease is a rare, inherited disease that causes the progressive degeneration of nerve cells in the brain.
Symptoms associated with HD:
-
Progressive disorder (voluntary and involuntary) in the hands:
-
Twitching of the hands
-
Difficulty manipulating small objects
-
-
Chorea:
-
It is a jerky, rapid, uncontrolled and irregular movement.
-
Disappear during sleep
-
-
Oral function difficulties:
-
Abnormal facial expression
-
Aspiration*, dysarthria**
-
-
Difficulty performing voluntary movements:
-
Akinesia***
-
Bradykinesia****
-
-
Behavior (irritability, anxiety, depression)
-
Cognitive (concertation, memory, plan, abstract thinking)
-
Difficulty maintaining adequate work performance
-
Verbal communication is spread until middle or late stage of HD
-
As HD progress, other symptoms can develop, including:
-
Depression
-
Chorea becomes more severe and may involve entire body
-
Hypertonia (rigid)
-
Disturbance in gait and balance
-
Sever difficulty in eye movements
-

* When something you swallow "goes down the wrong way" and enters your airway or lungs.
** A motor speech disorder in which the muscles that are used to produce speech are damaged, paralyzed, or weakened.
*** The loss of ability to move your muscles voluntarily.
**** Slowness of movement
Multiple sclerosis: is a progressive disease of the brain and spinal cord (CNS) that caused by an autoimmune system reaction to the myelin sheath characterized by relapses and remissions eventually it can affects the axons by scaring and cause permanent damage.
Symptoms: According to lesions, location characterized by unpredictable repeated relapsed followed by remission.
-
Paresthesia ,sensory loss in extremities
-
Diplopia: Double vision, causes a person to see two images of a single object, and visual loss in one eye.
-
Fatigue
-
Emotional lability
-
Cognitive deficits
In Later stages, other symptoms develop, including:
-
Paralysis of LE
-
Dysarthria:
-
Dysphagia
-
Severe visual impairment nystagmus
-
Ataxia:
-
Spasticity
-
Impaired cognition
Is an abnormal sensation of the skin (tingling, pricking, chilling, burning, numbness) with no apparent physical cause

Parkinson’s disease: Is a progressive neurodegenerative motor system disorder causing dysfunction in both voluntary and involuntary movements.
For more information, check this link: https://www.parkinsons.org.uk/information-and-support/what-parkinsons
Impairments of Parkinson:
-
Tremor (Resting, asymmetric, peripheral, UL>LL)
-
Mask face
-
Flex posture
-
Poor balance (frequent fall)
-
Shuffling gait
-
Freezing: Decreased arm movement, no trunk rotation
-
Difficulty in fine movement
-
Autonomic System (constipation, increased salivation)
-
Oral & speech impairment (quiet, ̄ decreased swallowing)
-
Cognitive Impairment
-
Fairly normal in early stages
-
Impairment (attention, learning, comprehension)
-
Dementia over 70 years
-
-
Behavior Change (depression, motivation, sleepless)
-
Movement:
-
Difficulty in initiating (akinesia)
-
Slowness of movement (bradykinesia)
-
Rigidity (hypertonicity) impairs smooth movement
-
1st the neck + shoulder
-
2nd the extremities + face
-
Is an involuntary rhythmic shaking movement in one or more parts of the body.
Dementia: is an (umbrella term) or general word used for progressive disorders of the brain:
Associated problems:
-
Memory loss
-
problems in Language, perception, thinking and judgment
Interfere with:
-
learning, communicating, relating and even caring for self
Most common types of dementia:
1. Alzheimer's Disease (AD)
-
AD makes up 50-70% of all dementias
2. Vascular Dementia
-
2nd most common type of dementia
-
It is caused by a lack of blood flow to the brain. It can be related to atherosclerotic disease or stroke
3. Lewy Body Dementia
-
It is caused by protein deposits in nerve cells. This interrupts chemical messages in the brain and causes memory loss and disorientation
-
Dementia with Lewy bodies shares many symptoms with PD and AD
4. Fronto-Temporal Dementia
-
It affects the front and side parts of the brain, which are the areas that control language and behavior. It is also known as Pick’s disease
Alzheimer’s disease:
-
A type of dementia
-
It is an irreversible, progressive brain disorder that slowly destroys memory and thinking skills and, eventually, the ability to carry out the simplest tasks.
Associated symptoms:
-
Predominately-early episodic memory difficulties
-
Difficulties with STM and recall / orientation
-
Problems in finding correct names
-
Word finding and ability to generate words
-
Significantly impaired social life
-
Significantly impaired occupational function
-
Gradual onset
-
Continuing decline: Not due to CNS or other
-
Conditions: (e.g., PD, delirium, schizophrenia)
To know more about the OT role with Alzheimer’s disease, check this file .
For more information about Alzheimer’s disease: watch this video: (https://www.youtube.com/watch?v=Eq_Er-tqPsA)
Polyneuropathy: It refers to the conditions that result when multiple peripheral nerves that carry messages to and from the brain and spinal cord to the rest of the body become damaged, which is also commonly called peripheral neuropathy.
Characterized by symmetrical, distal motor and sensory deficits that have a graded increase in severity distally.
Symptoms:
1. Motor symptoms:
-
Positive : Muscle cramps, fasciculations
-
Negative : early distal toe and ankle extensor weakness resulting in trips and falls
2. Sensory symptoms:
-
Prickling, searing, burning, and tight sensations
-
Paresthesia: Unpleasant sensations arising spontaneously without apparent stimulus
-
Hyperalgesia: Painful hypersensitivity to noxious stimuli
-
Neuropathic pain: cardinal feature of many neuropathies
-
Allodynia: perception of non-painful stimuli as painful
3. Autonomic dysfunction
-
Fainting spells (lose consciousness for a short amount of time )
-
Sweating reduced or excessive
-
Heat intolerance
-
Bladder- Bowel dysfunction
-
Orthostatic lightheadedness: is a form of low blood pressure that happens when you stand up from sitting or lying down which can make you feel dizzy or lightheaded.
Guillain Barre Syndrome (GBS): is a rare neurological disorder in which the body's immune system mistakenly attacks part of its peripheral nervous system—the network of nerves located outside of the brain and spinal cord.
Symptoms:
GBS usually affects the feet or hands first, before spreading to other parts of the body.
Early symptoms:
Symptoms of Guillain-Barré syndrome usually develop over hours or days and tend to start in the feet and hands before spreading to the arms and legs.
Including:
-
Numbness
-
Pins and needles
-
Muscle weakness
-
Pain during activities that shouldn't cause pain
-
Problems with balance and co-ordination: due to Nerve damage to the legs (peripheral neuropathy).
-
Supervision while standing, walking, and transferring.
-
These symptoms usually affect both sides of the body at the same time
Later symptoms:
The symptoms may continue to get worse over the next few days or weeks. Some people are only mildly affected, but others may have:
-
Difficulty walking without assistance
-
Inability to move the legs, arms and/or face (paralysis)
-
Difficulty breathing
-
Blurred or double vision
-
Difficulty speaking
-
Problems swallowing or chewing
-
Difficulty peeing, and constipation
-
Persistent and/or severe pain
GBS usually reaches its most severe point within 4 weeks. It may then remain stable for a few weeks or months before gradually improving.
Muscular dystrophy is a group of inherited diseases that damage and weaken your muscles over time. This damage and weakness is due to the lack of a protein called dystrophin, which is necessary for normal muscle function.
-
muscular dystrophy has different types according to the muscles that are affected. (check table 8)
Symptoms:
• Primary: Affect muscle structure
• Secondary: Affect musculoskeletal system
The symptoms Include:
-
Muscle weakness
-
Progressive muscle atrophy
-
Joints contracture
-
Poor balance (frequent falls)
-
Abnormal gait pattern (waddling)
-
Scoliosis: which is an abnormal curvature of your spine
-
Cardiomyopathy
-
Respiratory difficulty

Table 8
Myasthenia gravis is a chronic autoimmune, neuromuscular disease that causes weakness in the skeletal muscles that worsens after periods of activity and improves after periods of rest.
Symptoms:
-
Weakness of the eye muscles (called ocular myasthenia)
-
Drooping of one or both eyelids (ptosis)
-
Blurred or double vision (diplopia)
-
A change in facial expression
-
Difficulty swallowing
-
Shortness of breath
-
Impaired speech (dysarthria)
-
Weakness in the arms, hands, fingers, legs, and neck.
Sometimes the severe weakness of myasthenia gravis may cause respiratory failure, which requires immediate emergency medical care.
In occupational therapy, one of our focuses is the patient’s ability to participate effectively in their activities of daily living, comprising of their basic activities of daily living (ADLs), which include bathing, dressing, feeding, mobility, and grooming and instrumental activities of daily living (IADLs) which include caring for others, driving, financial management, home management/maintenance, meal preparation, and shopping.
Following a neurological disease, often individuals will notice difficulties in their ability to participate in their ADLs and IADLs. This may be due to cognitive, perceptual, sensory, or motor dysfunctions. Therefore, it’s necessary to assess the patient’s ability to perform ADLs and IADLs
Description: It is an 18-item, clinician-reported scale that assesses function of activities of daily living (ADL)in six areas including self-care, continence, mobility, transfers, communication, and cognition.
Scale: Each of the 18 items is graded on a scale of 1–7 based on level of independence in that item.
Scoring: FIM scores can be measured at admission to and discharge from inpatient rehabilitation
7= Complete independence (timely, safely)
6= Modified independence (extra time, devices)
Modified dependence:
5= Supervision (subject= 100%+)
4= Minimal assist (subject= 75%+)
3= Moderate assist (subject= 50%+)
Complete dependence
2= Maximal assist (subject= 25%+)
1= Total assist (subject= less than 25%)
For more information, check this link: https://strokengine.ca/en/assessments/functional-independence-measure-fim/
For a copy, check this file
Description: It is an ordinal scale used to measure performance in activities of daily living (ADLs).
Items: it includes 10 personal activities: feeding, personal toileting, bathing, dressing and undressing, getting on and off a toilet, controlling bladder, controlling bowel, moving from wheelchair to bed and returning, walking on level surface (or propelling a wheelchair if unable to walk) and ascending and descending stairs.
Scoring: Sum the patient's scores for each item. Total possible scores range from 0 – 20, with lower scores indicating increased disability.
If used to measure improvement after rehabilitation, changes of more than two points in the total score reflect a probable genuine change, and change on one item from fully dependent to independent is also likely to be reliable.
For a copy, check this file:
Description: is the most appropriate instrument to assess functional status as a measurement of the client’s ability to perform activities of daily living ADLs) independently.
Items: six items ( bathing, dressing, toileting, transferring, continence, and feeding).
Scoring: Clients are scored yes/no for independence in each of the six functions.
-
6 indicates full function.
-
4 indicates moderate impairment.
-
2 or less indicates severe functional impairment.
For a copy check this file:
Description: An observational assessment that allows for the simultaneous evaluation of motor and process skills and their effect on the ability of an individual to perform complex or instrumental and personal activities of daily living (IADL).
Number of items: 36 items (16 motor skills items, 20 process skills items)
Time to administer: 30-40 minutes
Scoring: uses a 4-point Likert scale to rate the client’s performance on 16 motor and 20 process skills.
How to obtain the tool?
The AMPS manual and software can be purchased online at https://www.amps-esiukandireland.com/amps
Description: it is a standardized assessment tool that seeks to provide information relating to an individual's ability to achieve successful and independent community living. Furthermore, this assessment tool has been proven to be effective for estimating the competence of individuals with a mental health diagnosis to live independently.
Subscales: it has five subscales, including:
-
Memory orientation (e.g., recall a shopping list)
-
Managing money (e.g., completing monetary calculations)
-
Managing home and transportation (e.g., using a telephone)
-
Health and safety (e.g., how to respond to an emergency situation)
-
Social adjustment (e.g., attitudes about interpersonal relationships)
Time to administer: it takes approximately 20 minutes to administer.
Scoring interpretation: The final score from the ILS determines if the individual falls within the category of low, moderate or high functioning for each subsection.
For a copy, check this file:
The American Spinal Injury Association Impairment Scale (ASIA)
Description: is a standardized neurological examination used to assess the sensory and motor levels which were affected by the spinal cord injury.
The scale has five classification levels, ranging from complete loss of neural function in the affected area to completely normal.
It is available but you should take permission to reprint using this link: https://asia-spinalinjury.org/international-standards-neurological-classification-sci-isncsci-worksheet/
Description: It’s used to measure muscle tone through measuring resistance during passive soft-tissue stretching and is used as a simple measure of spasticity.
Precaution: if the patient has subluxation, avoid testing the tone.
Scoring:
-
0 = no increase in muscle tone
-
1 = slight increase in muscle tone; manifested by a catch and release or by minimal resistance at the end of ROM.
-
1+= slight increase in muscle tone; manifested by a catch, followed by minimal resistance throughout the reminder (less than half) of the ROM.
-
2 = more marked increase in muscle tone through most of the ROM, but affected part/s easily moved.
-
3 = considerable increase in muscle tone, passive movement is difficult.
-
4 = affected part/s are rigid in flexion or extension.
For a copy, check this file:

Description: It is the amount of movement that is possible at a joint, and its measured using the goniometer.
As the ROM should be adequate to engage in meaningful and purposeful occupations, it should be measured to determine the limitation and how it interferes with the performance in areas of occupation.
Range of motion is either Passive or Active:
-
Passive range of motion (PROM): the joint is moved by the muscles that act on the joint.
-
Active range of motion (AROM): the joint is moved by an outside force.
Procedure of ROM:
-
Expose the area:
-
Explain to the patient and give instruction, placing the client as required.
-
-
Stabilization: stabilizing proximal joint to limit movement to joint being assessed.
-
Goniometer measurement:
-
Placement of axis, stationary, and movable arms.
-
Recording from starting degree position.
-
Precautions:
-
Joint inflammation
-
Taking medication for pain/ muscle relaxants
-
Osteoporosis/ hypermobility/ subluxation of joint
-
Hemophilia/ hematoma/ injury to soft tissue
-
Newly fracture
-
Prolong immobilization
-
Fragile bone condition
Contraindications:
-
Joint dislocation
-
Unhealed fracture
-
Immediately after surgery of soft tissue surrounding joint.
For more information about performing ROM for Upper extremity: check these videos:
Description: It is a procedure for the evaluation of muscle strength, based upon the effective performance of a movement in relation to the forces of gravity or manual resistance through the available Range of motion (ROM).
Scoring:
-
0 = no muscle contraction can be seen or felt
-
1 = contraction can be observed or felt, but there is no motion
-
-2= part moves through incomplete ROM with gravity minimized
-
2 = parts move through complete ROM with gravity minimized
-
+2= parts move through less than 50% of available ROM against gravity or through complete ROM with gravity minimized against slight resistance
-
-3= parts move through more than 50% of available ROM against gravity
-
3 = parts move through complete ROM against gravity
-
+3= parts move through complete ROM against gravity and slight resistance
-
4 = parts move through complete ROM against gravity and moderate resistance
-
5 = parts move through complete ROM against gravity and maximal resistance
For more detailed information about MMT: check this book:
Daniels and Worthingham's Muscle Testing: Techniques of Manual Examination and Performance Testing (Daniels & Worthington's Muscle Testing (Hislop)) 9th Edition
The book is Available in amazon: visit this link if you want to purchase it: https://www.amazon.com/Daniels-Worthinghams-Muscle-Testing-Worthingtons/dp/1455706159
-
Berg balance scale:
Description: 14-item scale designed to measure balance of the older adult in a clinical setting.
Time: 15-20 minutes
Scoring: A five-point ordinal scale, ranging from 0-4. “0” indicates the lowest level of function and “4” the highest level of function. Total Score = 56
Scoring interpretation:
41-56 = low fall risk
21-40 = medium fall risk
0 –20 = high fall risk
For more information, check this Video: https://www.youtube.com/watch?v=HBKXu9fHnuo&feature=emb_title
For a copy: Upload file name:
-
Functional Reach Test:
Description: It is a single item test developed as a quick screen for balance problems in older adults. It Measures the distance between the length of an outstretched arm in a maximal forward reach, while maintaining a fixed base of support, in standing. Modified Functional Reach Test (Adapted for individuals who are unable to stand)
Time: 1-2 minutes
Scoring:
-
A score of 6 inches or less indicates a significant increased risk for falls.
-
A score between 6-10 inches indicates a moderate risk for falls.
-
Minnesota Manual Dexterity Test:
Description: Standardized performance-based evaluation that measures simple, rapid hand-eye coordination and arm-hand dexterity (gross motor skills).
Time: Approximately 56 minutes
Availability: It should be purchased: it costs $200.00 Kit; $12.50 Additional score sheets using this link: https://lafayetteevaluation.com/products/minnesota-manual-dexterity
-
Purdue beg board test:
Description; It measures gross movement of the arm, hand and fingers, and fingertip dexterity.
For more information, check this link: https://strokengine.ca/en/assessments/purdue-pegboard-test-ppt/
To know how it done, check this video: https://www.youtube.com/watch?v=xXT9E4OY9tw
For the kit, it should be purchased using this link:
https://www.amazon.com/Lafayette-Instrument-12-3000-Purdue-Pegboard/dp/B003YR6SDE

-
Pinch strength: using pinch meter.
There are three types:
-
Tip- to tip: the pinch meter is placed between the tip of the thumb and the tip of the index finger.
-
Tripod (chuck): The pinch meter is placed between the pad of the thumb and pad of the index and middle fingers.
-
Lateral: The pinch meter is placed between the pad of the thumb and the lateral surface of the index finger.
For more information, visit hand therapy (assessment section)
Standardized assessment:
-
Test of Everyday Attention(TEA):
Description: It measures 3 aspects of attention—selective attention, sustained attention, and attention switching—using everyday materials.
Time: 45-60
To purchase, check this link: https://www.pearsonclinical.co.uk/Psychology/AdultCognitionNeuropsychologyandLanguage/AdultAttentionExecutiveFunction/TestofEverydayAttention(TEA)/TestofEverydayAttention(TEA).aspx
-
Short Blessed Test:
Description: A short tool to assess orientation, memory, concentration.
For a copy, check this file:
-
Neurobehavioral Cognitive status Screening Examination (COGNISTAT):
Description: it measures 10 subtests in areas of orientation, attention, comprehension, repetition, naming, construction, memory, calculation, similarities, and judgments.
Time: 20-25 minutes
To purchase, check this link: https://www.cognistat.com/cognistat-assessment-system-products-and-pricing
-
D2 Test of Attention:
Description: A paper and pencil test measures selective and sustained attention and visual scanning speed through asking the patient to cross out any letter "d" with two marks around above it or below it in any order.
To purchase, check this link: https://www.hogrefe.com/uk/shop/d2-test-of-attention.html
-
Contextual Memory Test:
Description: It assess memory capacity, strategy of use, and recall in adult clients with memory dysfunction, in which the patient tries to remember 20 objects related to one of two themes.
Time: 30-40 minutes
For more information, check this file:
-
Rivermead Behavioral Memory Test:
Description: It assesses memory skills necessary for everyday life including remembering names, faces, and appointments.
Time: 30-45 minutes
To purchase, check this link: https://www.pearsonclinical.ca/en/products/product-master/item-119.html
-
Mini-Mental Status Examination (MMSE):
Description: It is a widely used test of cognitive function among the elderly; it includes tests of orientation, attention, memory, language and visual-spatial skills. Total score: 30
For more information: check this file:
-
Montreal Cognitive Assessment (MoCA):
Description: it assesses short term memory, visuospatial abilities, executive functions, attention, concentration and working memory, language, and orientation.
Scoring interpretation:
Total score: 30
Normal= equal or more than 26/30
For a copy, check this file:
-
Loewenstein Occupational Therapy Cognitive Assessment (LOTCA):
Description: It measures basic cognitive skills required for everyday function including orientation, visual perceptual and psychomotor abilities, problem-solving skills and thinking operations.
Time: 30-45 minutes
To purchase: it costs $267.58 from AllegroMedical.com
For more information: visit this link: https://strokengine.ca/en/assessments/loewenstein-occupational-therapy-cognitive-assessment-lotca/
OR check this file:
-
Arnadottir OT-ADL Neurobehavioral evaluation (A-ONE):
Description: It is a standardized, performance-based measure that identifies the impact of neurobehavioral impairment on functional performance of ADL.
It comprised of two parts: (a) assessment of the individual’s independence in ADL tasks and the type of assistance required; and (b) identification of the type and severity of neurobehavioral impairment that is limiting the individual’s independence in these tasks.
Time: 25 minutes
Availability: it should be purchased: it costs $37.97 to $117.92 to buy the textbook that it is in (The Brain and Behavior: Assessing Cortical Dysfunction Through Activities of Daily Living by Guorun Arnadottir).
For more information: check this link: https://strokengine.ca/en/assessments/arnadottir-ot-adl-neurobehavioural-evaluation-a-one/
Or check this file:
Sensation screening: to screen superficial, deep, and mixed sensations.
-
Superficial sensation:
-
Light touch/ pressure: while using cotton or your finger
-
Pain: sharp / dull: using the pen
-
Temperature: using tubes
-
Deep sensation:
-
Proprioception: With the patient's eyes closed, test his/ her ability to determine the direction of movement as you move the big toe upward or downward.
-
Kinesthesia:
-
Tactile localization
-
Vibration: avoid doing it for those with seizures.
-
Mixed sensation:
-
Stereognosis: ask the patient to close his/ her both eyes and identify the object you placed in his/ her hand. EX: Place a coin or pen.
-
Graphasthesia: draw a number, letter, or shape on the palm of the patient’s hand with your fingertip, and then ask the patient to identify the number, letter, or shape.
Scoring:
NT: not tested
0: Absent, No response
1: decreased, delayed response
2: increased, exaggerated response
3: inconsistent response
4: intact, Normal response
Instructions:
-
Do it in a calm place
-
The patient should close his eyes
-
If the patient has one side affected, first you have to do it in the non-affected side to make the patient know how the feeling should be, then do it in the affected side.
-
You have to do each component 3 times.
-
If the patient has seizures, avoid doing vibration.
-
In tactile localization, avoid other touch in any other area than the area you are assessing.
For a copy, check this file:
Vision screening:
As the individuals with a moderate to severe TBI have a 1/3 chance to have a visual impairment. Common deficits include:
• Reduced visual acuity
• Visual field loss
Visual assessing components:
-
Oculomotor control: Oculomotor Control: Efficient movement of the eyes in a coordinated manner.
-
Ocular movements
-
Visual Tracking: hold a pen in front of the patient and instruct the patient not to move his head and follow the pen when you move it.
-
Visual Acuity: Snellen Board:
Instructions:
-
Client seated/standing 10’ away from Snellen chart.
-
Client reads chart from top to bottom (from largest letter to smallest), left to right.
-
Cover one eye first and read chart
-
Next cover opposite eye and read chart
-
Finally have client use both eyes and read chart
Standardized Norms:
“Normal” Distance Visual Acuity = 20/20
For more information: check this link: https://otassessments.wordpress.com/va/
-
Visual Field: instruct the patient to cover one eye then place a pen at the side of the patient’s head and ask the patient if he can see the pen while looking forward and without moving his/ her head.
-
Visual attention:
-
Letter cancelation: the patient is presented with a piece of paper that has various lines scattered across it and is asked to mark each of the lines. If the patient completely ignore all lines on the left side of the paper, then he/ she has left side neglect and vice versa.
-
Line bisection: is a quick measure to detect the presence of unilateral spatial neglect (USN). The patient must place a mark with a pencil through the center of a series of horizontal lines. If there is a deficit, The displacement of the bisection mark towards the side of the brain lesion is interpreted as a symptom of neglect.
Visual perceptual Standardized assessments:
-
The biVABA (The Brain Injury Visual Assessment Battery for Adults):
Description: designed to assess visual problems after Brain injury.
Its A collection of instruments to screen for visual processing impairments following brain injury. The intention of the battery is to find out whether and how visual processing impairments prevent or hinder participation in occupations.
To purchase, check this link: https://www.visabilities.com/bivaba.html
For more information: Check this file:
-
Developmental Test of Visual Perception–Adolescent and Adult (DTVP-A):
Description: is a battery of six subtests that measure different but interrelated visual-perceptual and visual-motor abilities. It is especially useful in the evaluation of the neuropsychological integrity of TBI and stroke patients where right-hemisphere function may be an issue.
Time: 25 minutes
To purchase, click here.
-
Motor Free Visual Perceptual Test (MVPT-4):
Description: It assess visual–perceptual ability without requiring a motor response from the examinee.
Time: 20-25 minutes
To purchase, check this link: https://www.wpspublish.com/mvpt-4-motor-free-visual-perception-test-4
-
Fatigue severity scale (FSS):
Description: Self-report questionnaire designed to evaluate the impact fatigue has on a patient.
Items: 9 statements
Scale: each statement has a scale of 7 (1 reflects strong disagreement with the statement, and 7 reflects strong agreement with the statement)
For a copy: Check this file :
-
Numeric Pain Rating Scale (NPRS):
Description: is a brief self- report questionnaire in which patients rate their pain intensity using an 11-point scale (10 indicates pain as bad as it can be and 0 indicates no pain).
For a copy, check this file:
-
Borg rating of perceived exertion:
Description: it measures physical activity intensity level.
Scale: 6-20 (6 indicates no exertion at all, 20 indicates maximal exertion)
For more information, check this file:
After using an appropriate assessment, we have to plan the intervention incorporating the client’s priorities and needs.
Reminder: Try to use meaningful and purposeful activities.
Most common used approaches in this area:
1. Biomechanical Frame Of Reference: It is based on the following assumptions as described by Dirette (2005):
-
Occupation can remediate the loss of ROM, strength and/ or endurance
-
By regaining ROM, strength and/or endurance, functional skills can be enabled
-
The body must rest, then work
-
A level of cognition is required to produce isolated/ coordinated movements
Dirette states that this FOR works to improve structural stability, AROM, PROM, muscle strength, peripheral edema and endurance through:
-
A graded increase in duration and intensity to increase endurance
-
Exercise via isometrics, active assistance, passive and active stretch, active motion, and progressive resistance to increase strength
-
AROM and occupation to maintain strength
-
PROM, AROM, active assistance range of motion (AAROM), scar prevention, orthosis, positioning, and occupation to increase ROM
-
Rest followed by stress to increase structural stability
Clinical application of this FOR:
It can be seen when working with a post-CVA client with subdued shoulder. To remediate this problem via biomechanical FOR, the therapist can work to improve positioning by using a sling. In addition, the therapist can stimulate the surrounding rotator cuff muscles as well as use PROM and AROM to help preserve and improve the ROM at the joint.
2. Rehabilitative Frame Of Reference: the assumptions that Dirette gives for this FOR are:
-
Independence can be reaching with compensation when deficits cannot be overcome
-
The environment, volition and habits of a person are an integral part of their motivation for a person to be independent. Independence
-
A certain level of cognitive and emotional skills ae required
This independence is achieved through Adaptive devices, orthotics, environmental modifications, wheelchair modifications, ambulatory aids, and/or safety education. (Dirette (2005).
Clinical application of this FOR:
It can be seen when working with a client with degenerative diseases that has led to a decreasing amount of strength and ROM in their hands. A person with this kind of dysfunction would have a difficulty with the ADL of dressing. To enable greater independence an adaptive devices such as dressing stick could be used.
3. Bobath Approach/ (NDT= Neuro-Developmental Treatment):
-
Is an advanced hands on approach to the examination and treatment of individuals with disturbances of function, movement, and postural control due to a lesion of the CNS.
-
Its goal is to normalize the tone and to facilitate voluntary and normal movement patterns that are modified at proximal key points of control (e.g. shoulder and pelvic girdle)
-
Principles of treatment:
-
Normalize muscle tone (for more information check normalizing tone section)
-
Inhibit primitive reflexes
-
Facilitate normal postural control
-
-
Techniques:
-
Handling
-
Weight bearing over the affected limb
-
Utilize positions that allow use of the affected limbs
-
Avoidance of sensory input that affect muscle tone
-
Clinical application of NDT:
It would be working to decrease tone and increase control in the UE with a post-CVA client. Through having the client perform weight shifts in a quadruped position, the synergist tone can be decreased in the arm to facilitate controlled movement.
4. Brunnstorm Approacch:
The Brunnstrom treatment approach is based around two principles:
1st Principle: Normal movement (how a healthy individual moves) requires muscles working together (synergistically) following damage to the CNS the muscles will not work as well together. During recovery muscles will start working together better.
2nd Principle: Following damage to the CNS, movement recovery follows a specific sequence. The sequence of recovery process is :
-
Immediately after the onset of injury there may be no "voluntary" movement.
-
Spasticity (increased muscle tone) appears, basic movement reflexes appear.
-
Patient begins to gain voluntary control over their reflexes. This may cause an increase in spasticity.
-
Basic movement patterns are developed. This leads to a reduction in spasticity.
As progress continues, more complex movement patterns are learnt and there is a further decrease in spasticity. -
Spasticity disappears and individual movements become possible and coordination approaches normal.
-
Normal function is restored.
5. Propioceptive Neuromuscular Facilitation (PNF) is the neurophysiological approach in which impulses from the periphery are facilitated to the central nervous system through the stimulation of sensory receptors present in muscles and around the joints.
The basic procedure used for PNF application is:
a. Resistance: To increase muscle strength, motor learning and motor control.
b. Irradiation and reinforcement: Assistance to weak muscle by surrounding strong muscles by spread of response to stimuli.
c. Manual contact: To increase awareness, to guide direction and to give resistance.
d. Body position and body mechanics: Guidance, control of motion, balance and stability.
e. Verbal stimulation (Commands): For guiding the patient about the movement.
f. Vision: For reinforcement and guiding motion
g. Traction and Approximation: For stimulation of proprioceptors in muscles and around joint
h. Stretch: Stretch may be quick or sustained. Quick stretch facilitates the muscle contraction
i. Timing: Promote normal timing and increase muscle contraction through “timing for emphasis”.
j. Patterns: Synergistic mass movements, components of functional normal motion in diagonal and spiral pattern.
For more information, check this file:
1. Motor relearning program:
Is a rehabilitation training focusing on motor function recovery post central nervous system injury.
-
Recovery mechanisms based on the principle of Brain Plasticity (neural plasticity): Damaged brain repairs itself by means of physiologic responses.)
-
It influenced by:
-
Environment
-
Repetition of tasks
-
Motivation
-
-
Techniques:
-
Verbal and visual feedback
-
Instruction
-
Manual quidance
-
Steps:
-
Analysis of function:
-
Observation
-
Comparison
-
Analysis
-
-
Practice of missing component:
-
Explanation and instruction
-
Practice (verbal feedback and manual guidance)
-
-
Practice of activity:
-
Explanation and instruction
-
Practice
-
Progression(grading up), increase complexity, add variety, decrease feedback and guidance
-
-
Transfer of learning:
-
Opportunity of practice
-
Consistency of practice
-
Involvement of therapist or caregiver
-
Positive reinforcement
-
Stimulating environment
-
Clinical application:
It can be seen when working with child on handwriting. At an early stage, the use of stencils or guiding with hand over hand would be used to learn the idea of the movements. This would be followed by the use of handwriting paper, which provides visual cues and feedback as the movement are created more independently. As the movements are practice, with feedback from both visual cues and from the therapist a child develops the motor movements needed for the skill.
2. Task oriented Approach (TOA):
It is based on a systems model of motor behavior and emphasizes the interrelatedness of client, task, and environment factors on motor performance.
-
It enables the patient to obtain motor recovery through:
-
Occupation based and client centered activities
-
Teaching general strategies for solving motor problems
-
Occupational performance using real objects, environment and meaningful occupations.
-
-
The approach assumes that:
(1) Functional tasks organize motor behavior
(2) Motor behavior is the result of the interaction of the person with the environment
(3) Occupational performance observed after central nervous system damage reflects the person’s attempt to achieve task goals
(4) Exploration and practice are the means by which people find solutions to motor problems
For more information, check this file:
The Person-Environment-Occupation (PEO) model:
It is a model that emphasizes occupational performance shaped by the interaction between person, environment, and occupation.
-
The person domain includes role, self-concept, cultural background, personality, health, cognition, physical performance, and sensory capabilities.
-
The environmental domain includes physical, cultural, institutional, social, and socio-economic environment.
-
The occupation refers to the groups of tasks that a person engages in and meets his/her self-maintenance, expression and fulfillment.
The three domains are dependent and affected by each other. In this model, the overlapping area of the three domains shapes occupational performance dynamically, and also represents the level of congruence of the interaction between the person, environment and occupation. With the higher level of congruence, the quality of occupational performance is increased and vice versa.
NOTE: When occupational therapist plan an intervention plan, he should look at the person holistically, environment, and occupation to achieve occupational performance and reach the goals.
Check this figure:

Decreased or impaired consciousness or alertness refers to decreased responsiveness to external stimuli. Diseases that damage the brain cells can cause impaired consciousness, such as Traumatic Brain injury (TBI). Coma is the most severe level of consciousness impairment.
Our role as occupational therapists with patients who are in Coma or have decreased consciousness is to increase the level of awareness through Sensory Stimulation:
-
Intervention for clients who emerged from coma should start as soon as possible they are medically stable.
-
The goal of intervention is to increase the client’s level of awareness (arousal) with controlled sensory input, especially for TBI patients, Including:
-
Visual Example: light can be used to elicit eye opening and visual tracking.
-
Auditory: Example: familiar music can facilitate autonomic responses (e.g. change in blood pressure)
-
Tactile: Example: any texture can be used to elicit eye opening.
-
Olfactory: Example: (variety of scents) can elicit head turning.
-
Gustatory: Example: through presentation of taste to lips, tongue using a cotton swab (Salty, sweet, bitter, and sour taste).
Note: the most effective types of sensory stimulants are those that have personal meaning to the client, such as favorite smell, or song.
For more information about occupational therapy role with TBI patient, check this video: https://www.youtube.com/watch?v=0pIY8ESjHtQ
For more information about the effectiveness of sensory stimulation, check this article:
Cranial nerves dysfunction:
The cranial nerves are 12 pairs of nerves that emerge from the brain and are responsible for providing motor and sensory functions.
Check this file that includes the 12 nerves, their classification, and their function, and how to assess each nerve.
Cranial nerve issues can affect a motor nerve, called cranial nerve palsy, or affect a sensory nerve, causing pain or diminished sensation. Individuals with a cranial nerve disorder may suffer from symptoms that include:
-
Intense pain, vertigo, hearing loss, weakness or paralysis. These disorders can also affect smell, taste, facial expression, speech, swallowing, and muscles of the neck.
Most common Cranial nerves Disorders:
Trigeminal Neuralgia:
Is a disorder of the fifth cranial nerve, the trigeminal nerve, which is a large nerve that carries sensation from the face to the brain and controls motor functions such as biting and chewing.
Facial pain
Symptoms include Pain that usually localized in one side of the face and is felt in contact of a light touch or a sound. It's usually triggered by the following activities:
-
brushing teeth
-
shaving
-
rubbing
-
touching the painful area of the face
-
putting on makeup
-
eating or drinking
-
speaking
-
being exposed to the wind
-
pain in the cheek, jaw, teeth, gums, and lips
-
pain in one side of the face
-
tingling or numbness in the face before starting to feel pain
Occupational therapy treatment aims at reducing pain and improve the ability to carry on with the activities of daily living (ADLs) by using:
-
Relaxation techniques such as deep breathing exercises.
-
Functional Activities for problems associated with ADLs.
-
individual's education on diet, management of sleep, and rest.
-
Advice on how to avoid using cold water for drinking and washing their face but also chewing with the non-affected side.
Facial/Bell’s palsy:
Bell’s palsy is a condition that causes a temporary weakness or paralysis of the muscles in the face. It can occur when the nerve that controls the facial muscles becomes inflamed, swollen, or compressed.
Symptoms include:
-
Droopy appearance on one side of the face and the inability to open or close your eye on the affected side.
-
A drooping eyelid or corner of the mouth
-
Drooling
-
A dry mouth
-
A loss of taste
-
Eye irritation, such as dryness or more tears
Occupational therapy treatment include:
-
Facial massage:
-
Put left index and middle fingers under the chin and use the right index and middle fingers to massage the cheeks in circular motion
-
With index and middle fingers, massage the face from the forehead to the cheeks on arch move ( with medium Pressure)
-
Passive stimulation: ex: face scrubbing for sensation
-
For drooling: blowing exercise: give the patient a straw to blow:
-
Blow in a cup of juice ( grade up with thick juice)
-
Blow on a paper (grade up by pressing on the straw)
-
-
Home program exercises (when click on home program go to home program (facial palsy home program) section )
Cognitive dysfunction refers to deficits in attention, verbal and nonverbal learning, short-term and working memory, visual and auditory processing, problem solving, processing speed, and motor functioning.
Cognitive impairment is not caused by any one disease or condition, nor is it limited to a specific age group. Alzheimer’s disease and other dementias in addition to conditions such as stroke, traumatic brain injury, and developmental disabilities, can cause cognitive impairment.
Occupational therapist provides Cognitive rehabilitation through:
-
Intervention should be implemented through functional ADLs and IADLs.
-
EX: engaging those patients with cognitive problems in activities they need to participate in everyday life.
-
-
Providing assistive technologies
Example of interventions used for memory:
1. Memory strategies:
-
External Memory Strategies: Tools which help compensate for memory impairment. When effectively used they can reduce day-today memory problems, including:
-
Daily Planner/ Notepad: Used to record/check information across several categories such as appointments, “things to do”, contact details, personal information and general note taking
-
Calendars: Used to record and check events across time (e.g. birthdays, future activities)
-
Laptops, smart phones, tablets and other electronic devices: using various Apps or software programs which can be used to record or check information, appointments and events; link information across devices and set alarms to help recall important events. Trials for functionality of devices , apps and software prior to purchase are recommended.
-
Whiteboards: Used to provide a larger and more visual representation of a daily planner/ notepad but over a much shorter period of time.
-
Lists / Checklists: Lists are used to record steps for specific routines (e.g. bedtime routine) or lists of items (e.g.shopping list)
-
Medication blister packets from a Pharmacist: The most common pre- packaged version of medication blister packs brands available is a “Webster Pack”. These are available from a Pharmacy and must be organized by your GP
-
Medication dosette boxes: Dosette boxes can also be used to organise medications. These are used to sort your own medication yourself, however some Pharmacists will pre-pack medication into suitable dosette boxes.
-
2. Environmental memory strategies: involve modifying the environment or the way you interact with the environment. They can be used in conjunction with external memory strategies to help remind you to use specific external strategies, including:
-
Having a Routine: Can help with memory as tasks can become a habit after some time (e.g. writing your daily list of things to do with your morning coffee first thing in the morning)
-
Everything having a place: Effective use of this strategy will reduce need to “go looking for” or misplacing items (e.g. hook at front door for keys)
-
Keeping things in sight: By placing external memory strategies or various items in certain places that are used as visual cues to complete a task (e.g. placing pegs on the counter to remind you that the clothes are on the line) Labelling drawers and cupboards with contents can help to prevent clutter while reminding of the existence of some items. This can help to prevent over purchasing
-
Designating a point of organization: Using a desk and/or computer/filing cabinet to organise various affairs (e.g. bills)
-
Avoiding a cluttered environment: A cluttered or untidy environment may cause things to be lost more easily
3. Internal memory strategies: they can be described as focusing your attention in a particular way and being mindful of certain information.
-
Mental Imagery/ Visualization:
-
Forming an internal ‘visual image’ to assist with learning and recall “visualising,” “seeing in the mind's eye,” “hearing in the head,” “imagining the feel/smell/taste of”
-
Remembering an experience without an external prompt
-
Copying or reconstructing past experiences or imagining / anticipating possible future experiences
-
Examples for Visualization:
Example/Exercise 1: Try to visualise where you have breakfast; the table, the plate, the cutlery, the food, what it smells like, moving your arms to put the food in your mouth, what it taste like, what you usually hear i.e. kids, TV, birds etc.
Example/Exercise 2: Rehearse in your mind or visualise your morning routine and all the tasks involved. Break each task down as much as you require to be able to complete the task yourself in your mind, that is, if you experience difficulty putting your top on, break that task down to every step that you would need to do in real life.
-
Association:
-
This involves relating what you want to learn with something you already know
-
It’s the process of forming a link between visual information and verbal information, new information and prior knowledge and environmental cues and intended actions
-
Examples for Association:
Example/ Exercise 1: Associate in your mind the person you have just been introduced to with another person you already know with the same name, whether it be a friend, family member or famous person,
Example / Exercise 2: If you are having trouble remembering something, it can be helpful to think of as much related information to the situation as possible. This increases the chance that you will trigger an association and remember what you were trying to remember.
-
Categorization/chunking: Refers to organizing or grouping separate pieces of information together.
Examples for Categorization:
Example:/ Exercise: Breaking your lengthy shopping list up into smaller categories “fruit and vegetables”, “dairy”, “cleaning products”, “meats” etc.
-
Repetition/Rote learning: Trying to learn something that isn't meaningful by repeating it over and over
-
4 pillars of a healthy lifestyle: A balanced and healthy lifestyle is important for maintaining mental performance including memory. This can be accomplished through consistent exercise, good diet, adequate sleep and maintaining stress. It is important to understand that this balanced lifestyle is specific to a person’s standards and capacities, as each person is an individual and every brain injury is unique. The 4 pillars are:
-
Exercise helps by improving blood circulation, thus supplying extra oxygen to the brain and promoting growth of new brain cells.
-
By maintaining a good diet you can enhance your concentration and memory
-
Quality sleep helps you think more clearly, be more alert and function at your best in all areas; physical, mental and emotional.
-
Chronically high levels of stress are not only bad for blood pressure, cholesterol and other physical problems, but also wears away at brain fitness and overall memory performance.
For more detailed activities for each cognitive skills, check this file:
More about occupational therapy role with Alzheimer’s disease, check this file:
Apraxia:
It is a neuropsychological deficit that can affect stroke patients. It refers to ’disorders of the execution of learned movement which cannot be accounted for by either weakness, incoordination, or sensory loss, or by incomprehension of or inattention to command.
There are several kinds of apraxia, which may occur alone or together. The most common is buccofacial or orofacial apraxia, which causes the inability to carry out facial movements on command such as licking lips, whistling, coughing, or winking. Other types of apraxia include limb-kinetic apraxia (the inability to make fine, precise movements with an arm or leg), ideomotor apraxia (the inability to make the proper movement in response to a verbal command), ideational apraxia (the inability to coordinate activities with multiple, sequential movements, such as dressing, eating, and bathing), verbal apraxia (difficulty coordinating mouth and speech movements), constructional apraxia (the inability to copy, draw, or construct simple figures), and oculomotor apraxia (difficulty moving the eyes on command).
Apraxia intervention techniques:
-
Strategy training in daily living activities: this technique teaches internal (for example, the patient is taught to verbalise and implement the task steps at the same time) or external (for example, when aids are used to overcome a functional barrier) compensatory strategies that enable a functional task to be completed. These strategies will not have been used prior to the stroke.
-
Sensory stimulation: stimulations including deep pressure, sharp and soft touch are applied to the patients' limbs.
-
Proprioceptive stimulation: the patient leans on and puts weight through their upper and lower limbs;
-
Cueing, verbal or physical prompts: given to enable each stage of the task to be completed;
-
Chaining (forward or backward): the task is broken down into its component parts. Using backward chaining the task is completed with facilitation from the therapist apart from the final component, which the patient carries out unaided. If successful next time further steps are introduced. Forward chaining is the reverse of backward chaining.
For more information, check this article:
Perceptual deficits:
For those patients with perceptual deficits, Occupational Therapist help them through:
-
Rehabilitative interventions: EX: impairment for figure ground perception might be treated through repeated practice of locating objects against a similar background. (finding a spoon in a drawer of similar stainless steel utensils)
-
Compensatory intervention: EX: impairment for figure ground perception can be compensated through arranging the kitchen the kitchen drawers so the utensils are categorized based on color.
For more detailed activities for each perceptual skill: check this file:
Unilateral neglect:
Unilateral neglect is an attention disorder that arises as a result of injury to the cerebral cortex [1]. Unilateral neglect is also commonly known as contralateral neglect, hemispatial neglect, visuospatial neglect, spatial neglect, or hemineglect.
In unilateral neglect, patients fail to report, respond or orient to meaningful stimuli presented on the affected side. In most cases, the right parietal cortex is injured and the left side of the body and/or space is/are ignored.
To help those patient with unilateral neglect, Occupational therapist should:
-
Try to incorporate the neglected side during the session through:
-
Have a chair next to the bed on the neglected side as this encourages the patient to look in your direction.
-
As you talk to him\her, hold neglected hand, touch patient’s arm; make contact with the patient, helping the patient to become more aware of that side.
-
If the patient have difficulty turning their head in your direction, gently place your hand on his\her chin and slowly help him\her turn their head toward you.
-
Be far enough for his\her eyes to meet yours.
-
Provide Home program: (give the patient/ caregiver some instruction to follow through daily tasks).
Ataxia:
It’s a common motor dysfunction that occurs as a result of damage to the cerebellum or to the neural pathways leading to and from the cerebellum.
Occupational therapy treatment:
-
Frenkel’s exercises, check this file:
-
Environmental adaptations
-
Assistive technologies
Case study for a patient with ataxia:
Decreased Range of motion (ROM):
Occupational therapist increase ROM gradually, through passive OR active range of motion.
Passive and active range of motion Very important component of the OT treatment and is very important for both patient and family to start early in disease process and perform it daily
-
Purposes:
1. To prevent contractures (predominately in the shoulder and/or wrist/hand)
2. To decrease pain (from contracture, spasticity, cramping)
3. To facilitate and increase respiratory function
Abnormal tone:
The occupational therapist try to normalize muscle tone through using Neurodevelopmental Theory (NDT) techniques.
-
Hypertonic: inhibition techniques:
-
Slow brushing
-
Slow Range of motion
-
Weight bearing on the affected limb: Check this video: https://www.youtube.com/watch?v=DXH9rrqmfBE
-
Splinting
-
Muscle stretching: Precaution: should not be more than 90 degrees and should be done slowly.
-
Muscle stretching steps:
1- abduct the shoulder 90
2- extend the elbow in pronation
3- extend the thumb
4- extend finger
5- extend the wrist
6- compress for 10 seconds.
Check this video: https://www.youtube.com/watch?v=q2L3fgqyyQ4
-
Hypotonic: Facilitation techniques:
-
Fast ROM
-
Quick brushing
-
Quick tapping: check this video: https://www.youtube.com/watch?v=4b2UiVTlNLw&feature=youtube_gdata_player
-
Joint compression: through putting one hand above the joint for support and the other hand below the joint to push on.
-
Icing: watch this video: https://www.youtube.com/watch?v=nE7HcZqMEgs
-
Impaired sensation:
Sensory intervention techniques:
1. Tabletop touch therapy:
-
Let the patient to gather together objects with different textures and place them onto a table in front of him.
-
Then, without looking at the objects, let him to pick them up and feel them.
-
Let him try to distinguish the difference between textures.
Some examples of objects to grab are soft scarves, rough sandpaper, fluffy cotton balls, rough Velcro, and cool silverware.
2. Texture Hunting
-
Let the patient to fill a bowl with uncooked rice (anything from sensory box) and bury different textured objects in it, like marbles, coins, Velcro strips, cotton balls, etc.
-
Then, let him to reach his hand into the bowl and try to find the objects without looking.
3. Texture Handling
-
Place different objects in patient’s hand with his eyes open.
-
Let him Sense how these objects feel.
-
Once he has gone through all the objects and observed how they feel, let him performs the exercise again with his eyes closed.
-
Inform the patient to put all his focus into feeling each object to emphasize that connection in his mind.
Note: Let the patient note any difference between how the objects feel with his eyes open or closed.
4. Temperature Differentiation: This exercise is particularly beneficial to stroke survivors who have trouble feeling heat or cold.
-
Le the patient to soak a cloth in cold water and soak another cloth in hot (but not scalding) water.
-
Then place the cold cloth on his arm. Inform the patient to try sensing what that feels like.
-
After 30 seconds, switch the cold cloth with the warm cloth. While letting the patient to try sensing the difference in temperature.
-
Then, let the patient to close his eyes. And you have to place one cloth on his arm and try to determine if he is feeling heat or cold.
-
Repeat this exercise back and forth alternating from hot to cold.
5. Sensory Locating
-
Let the patient close his eyes
-
Place the patient’s hand somewhere on his arm.
-
Then, let him point to the area that he think you touched.
-
If he did not point to the correct area, move the patient’s hand. Then, open your eyes to visually absorb the information.
Pain:
As pain is mostly common among stroke patient, we as occupational therapists have a critical role in managing pain through:
-
Physical agent modalities (such as hot pack)
-
Positioning
Shoulder subluxation:
Shoulder subluxation: Occurs in around (30%- 80%) of persons post stroke with flaccid upper extremity.
To prevent subluxation, the occupational therapist should focus on:
-
Achieving trunk alignment
-
Scapula stability in a position of upward rotation
-
Passive range of motion: Recommended to avoid shoulder ranging past 90 degrees of flexion and abduction: Emphasis on external rotation and abduction as tolerated
-
Slings and straps: some benefit to prevent shoulder subluxation however little evidence for pain reduction
Management:
-
Facilitation of the muscles using facilitation techniques
-
Strengthening muscles of the joint. EX: rotator cuff muscles
Impaired balance/ trunk control:
Occupational therapist improve balance/ trunk control through:
-
Normal body alignment
-
Trunk movements/postural control: Facilitate rolling
-
Trunk Rotation (while supine): Passively move shoulder and hip in opposite directions. Check this video: https://www.youtube.com/watch?v=iWFWITdy1TA
-
Balance training through:
-
Facilitate static righting* in sitting
-
Facilitate Shifting: shift the weight forward and backwards; or from side to side( one hip to the other).
-
* Reflex that corrects the orientation of the body when its taken out of normal upright position.
Bed Mobility:
Note: always the therapist should be on the side along with middle of the patient’s body for safety. The therapist can give assistance in all these movements.
-
Rolling: Note: if the trunk is weak, the therapist gives assistance either from the knee or both the knee and shoulder.
-
Roll from the good side to the affected side
-
Roll from the affected side to the good side: the patient use the good hand to move the affected side.
-
-
Rocking the same movement of rolling but move the patient forward and backward repeatedly to strengthen the muscles.
-
Bridging: to strengthen the back muscles:
-
While in supine position let the patient lefts himself (the back) from the legs.
-
-
Scooting in bed: bridging then move with the bridged body.
-
Coming up to sitting:
-
Roll from the affected side to the normal side
-
Lower the legs
-
Lefts the upper body using the normal arm.
-
Transfers
Types:
Supine to sit/ Sit to stand/ stand pivot/ sliding board transfer/ Bed to chair/ wheelchair to toilet/ wheelchair to tub (shower)
-
For more information about the transfer techniques, check this file:
After an injury, most of the patients lost the ability to perform their Activities of daily living (ADL)/ Instrumental activities of daily living (IADL). Occupational therapist has to train the patient to perform the activity either by adapting the way of performing or using an adaptive equipment (if the patient reached plateau). For some patient who are able to perform the activity in the same way they were performing prior injury, occupational therapist can retrain them to perform it in the same manner.
ADLs / functional training:
-
Training in Self-care/ leisure and other areas.
-
For training, First you have to assess the skills to ensure that the patient is able to learn and improve.
-
Most common ADL training:
-
Dressing: EX: for hemiplegic patient use unilateral dressing technique (UE+LE)
-
Toilet training: either :
-
Commode chair
-
Sliding board transfer
-
-
Bathing: train the skills: EX : for polyneuropathy patients have sensory and balance problems:
-
Bathing training mostly while sitting for safety
-
Supervision for safety
-
How to know water temperature
-
-
Evaluate, recommend, and train for using Adaptive equipment:
Note:
-
We go for adaptive equipment if the patient reached plateau and there is no more progress
-
We have to consider the financial ability of the patient and his cognitive level.
To know more about the needed adaptive equipment, check assistive technology area
For those patients whose home environments restrict them to perform their activities, Occupational therapist needs to assess their homes and provide them with the needed modifications. As well as those patients who reached plateau or reached their maximum functional level, Home assessment should be done for them.
Home Assessment
It should be close to the date of discharge but not at discharge.
-
The occupational therapist should assess:
-
Patient’s capacity to perform usual activities
-
The Needs of the patient/ caregiver
-
Home safety environment
-
Risk of falls
-
Environmental barriers
-
Community access
-
For those patient who values work, occupational therapists help them through:
-
Community re-integration (vocational)
Pressure sores:
Pressure sores are areas of damaged skin caused by staying in one position for too long. They commonly form where your bones are close to your skin, such as your ankles, back, elbows, heels and hips.
Occupational therapist has to prevent Pressure sores through:
Educate the patient and the caregiver to:
-
Inspect the skin daily using mirror
-
Protecting vulnerable areas from shearing, moisture, and heat
-
Relieving and eliminating pressure points through Weight shifting every 30-60 minutes to relief pressure
-
Example: A Quadriplegia with 3+ shoulder and elbow strength pressure relief is done by leaning the trunk forward over the feet.
-
Push up using Upper Extremities.
-
Deep Vein Thrombosis (DVT)
DVT: is a serious condition that occurs when a blood clot forms in a vein located deep inside your body.
Occupational therapists manage DVT through:
-
Massaging
-
Compression stocking
-
Exercises
Orthostatic Hypotension:
Symptoms: dizziness, nausea and loss of consciousness.
Management: Recline quickly and if sitting in a wheelchair should be tipped back with legs elevated until symptoms subside.
Autonomic dysreflexia:
It is reflex action to any stimulus (e.g., bladder) in which there is a sudden onset of excessively high blood pressure and seen in spinal cord injuries above T6 level.
It occurs when something happens to the body below the level of the injury. This can be a pain or irritant (such as tight clothing or something pinching your skin) or a normal function that the body may not notice (such as having a full bladder and needing to urinate). These situations trigger an automatic reaction that causes the blood pressure to go up. As the blood pressure goes up, the heartbeat slows and may become irregular. The body cannot restore the blood pressure to normal because of the spinal cord damage. The only way to return things to normal is to change the situation—for example, by removing tight clothing or emptying the bladder.
Symptoms: immediate pounding headache, anxiety, perspiration, flushing, chills, nasal congestion, paroxysmal hypertension and bradycardia (slow heart rate).
Management: Occupational therapist should place the patient upright and remove thing that are restrictive. Also, Occupational therapist needs to monitor the patient (e.g. monitor urinary catheter for any blockage or twisting.
Spasticity management
It’s a motor disorder characterized by a velocity-dependent* increase in muscle tone due to a quick passive stretch, characterized by increased resistance to passive motion and involuntary muscle contractions”
*It’s a stretch reflex that is only elicited by the examiner’s rapid passive stretch.
-
To assess the spasticity: use Modified Ashworth scale
-
To manage:
-
Splinting and Casting : For more information, check Assistive technology area
-
Stretching the spastic limb:
-
As an example: how to stretch spastic Upper limb:
-
Abduct the shoulder
-
Slowly rotate the shoulder
-
Stabilize the elbow
-
Hold the wrist at the sides
-
Simultaneously extend the elbow and pronate the forearm
-
Extend fingers
-
-
To release spastic finger flexor: Check this video: https://www.youtube.com/watch?v=FhK5jUSx7oc
-
-
Home program exercises (check home program section)
Customizing splints:
The importance:
-
Maintain constant joint positioning with Static lengthening of muscle
-
Prevent contracture
-
Types of splints:
-
Functional Splints:
-
C-Splint: Positions thumb and index to compensate for thenar atrophy and to allow performance of fine motor tasks.
-
Thumb Spica Splint: provides stability of thumb for fine motor tasks
-
Wrist Cock-up Splint: To compensate for wrist drop and allow the patient to perform gross grasp task with wrist extensor muscle atrophy.
-
-
Contracture prevention splints: Resting hand splint and anti-spasticity ball splints.
-
For more information about splints check hand therapy and assistive technology areas
-
Mirror Therapy:
It is a therapeutic approach that uses a mirror box to regenerate neural networks that control limbs and other parts of the body.
-
The principle behind it is that a mirror box utilizes mirrors to give the impression to the user’s brain that they are moving an affected limb. So the patient performs exercises with an unaffected limb but because of the reflective surfaces inside the box, it appears as though the affected limb is being exercised.
-
How it’s done:
-
The mirror is situated on a table in front of the patient, and separates the left and right upper extremities.
-
The patient places his or her hands on the appropriate side of the central mirror, with the affected limb obscured by the mirror box itself.
-
The patient has to look at the reflection in the mirror. (fully attended)
-
-
Mirror Therapy session: check this video https://www.youtube.com/watch?v=1BnsQO7a4Og
Joint mobilization:
As an example: Scapula mobility:
-
Used for:
-
Hypertonic
-
Pain
-
Spasim
-
Steps:
-
Make the patient lie on the side
-
Put a pillow between you and the patient
-
Hold the acromion process and inferior angel of scapula
-
Then move the scapula in these motions:
-
Elevation/ Depression
-
Protraction (Abduction)/ Retraction (Adduction)
-
Upward rotation/ downward rotation
-
Winging
-
Check this video to know how to do Scapular Mobilizations to increase scapular mobility: https://www.youtube.com/watch?v=2mnasAQFMwg
For home program exercises, check this video:
-
Try to place objects on the neglected side such as the phone, TV remote control, glass of water or other necessities to encourage them look and reach for objects on that side.
-
The medicine or other important necessities should be placed in the good side.
Energy conservation refers to adapting the way you carry out your day-to-day activities, at work, rest and play to manage fatigue.
The weaker the patient becomes the more crucial energy conservation becomes.
Basic principles to apply:
1. Prioritize each day what you truly want to accomplish each day. Save your energy for the activities which are truly meaningful to you.
2. Identify what is not important. Eliminate it or have someone else accomplish it
3. Place rest breaks between each activity or within each activity between segments
4. Rearrange your activity and your environment so that everything is close at hand to require the least energy consumption
5. Realize that you only have so much energy available for each day. It is like a bank account in which only withdrawals are made
6. Listen closely to your body. If your body tells you that you need a rest break, then you need a rest break
7. If the activities of the day leave you tired the next day, then you have done too much and need to learn to scale back your activities
To apply the basic principles into daily activities, check these files:
Family/Caregiver education should start immediately as they are an integral part of the intervention team.
It includes:
-
Educate the caregiver about the condition and prognosis
-
Educate the caregiver about the affected ADLs and IADLs and the patient’s level in performing them
-
Educate the caregiver about the level of assistance needed while making sure that the patient is a primary participant in activities, and never try to perform everything for them.
-
Educate the caregiver about the environmental modifications or adaptive equipment needed (if necessary)
-
Training the caregiver ( ex: transfer)
Shoulder Arc
Description:
-
Designed to rehabilitate and improve ROM of the user's shoulder.
-
Constructed with a strong and durable hardened aluminum base that can be easily attached to a table top.
-
Includes 36-inch long, 29-inch high ROM tubing, and 24 colored movable tabs for ROM activities.
-
The shoulder arc provides customized rehabilitation programming for users.
-
Choice of a single arc or double-curved arc design.
Price: $465.29
To purchase, Check this link: https://www.rehabmart.com/product/shoulder-arcs-21794.html
Stacking Cones
Description:
-
It can be used to improve hand-eye coordination, sequencing, upper extremity exercise, color identification, and counting activities.
-
Stacking cones are convenient and versatile for easy use.
-
Washable, non-toxic design is durable and hygienic.
Price: $207.08
To purchase, check this link: https://www.rehabmart.com/product/rolyan-stacking-cones-14612.html
Therapy Ball (non-weighted)
Description:
-
It can be used to promote stability and improve dynamic sitting balance.
Price: $34.31
To purchase, check this link: https://www.rehabmart.com/product/stability-exercise-ball-with-pump-25445.html
Thera-putty (Weighted)
Description:
-
It can be used to develop finger dexterity, hand strength, and grip.
Price: $36.42
To purchase, check this link: https://www.rehabmart.com/product/cando-scented-theraputty-21630.html
Pronation/ Supination wrist exercise wheel
Description:
-
It exercises muscles in the wrist, forearm and shoulder of individuals recovering from surgery or injury.
Price: $50.00
To purchase, check this link: https://www.fab-ent.com/exercise/wrists-shoulder/cando-pronation-supination-wrist-exercis wheel/#:~:text=The%20CanDo%20Pronation%2FSupination%20Wrist,recovering%20from%20surgery%20or%20injury.
Shoulder Finger Ladder
Description:
-
Used to stretch, strengthen, and improve range of motion in the wrist, elbow, and shoulder.
Price: $126.56
To purchase, check this link: https://www.rehabmart.com/product/shoulder-finger-ladders-21808.html
Cuff Weights
Description:
-
Designed to be stronger and more durable, helping add resistance to exercise to build stronger muscles.
-
Weight range from 0.25 lbs to 25 lbs.
-
Velcro strap and ergonomic design to ensure snug, secure fit.
-
Color-coded for easy identification.
Price: $43,41
To purchase, check this link: https://www.rehabmart.com/product/original-cuffehabilitation-weight-single-weight-and-sets-21602.html
Graded Pinch finger exerciser set
Description:
-
Helps to improve the strength and coordination of the patient's fingers.
-
Pins vary in resistance and are color-coded for quick and easy selection.
-
Vertical and horizontal rods promote greater range of motion and adaptable therapy.
-
Set includes a range of pins and several rods for versatile rehabilitation.
Price: $243.74
To purchase, check this link: https://www.rehabmart.com/product/graded-pinch-exerciser-21617.html
Bolt board (screws)
Description:
-
Two-tiered, lacquered wooden platform provides added complexity during therapy
-
Helps increase dexterity and strength to the wrist, hand, and fingers
-
Bolts progress in diameter sizes from ¼ inches to ½ inches
-
Assorted nuts and washers included
-
Bottom of the base has a felt-covering to reduce tabletop damage
Price: $147.98
To purchase, check this link: https://www.rehabmart.com/product/twotiered-horizontal-bolt-board-14627.html
Hand gripper/ Hand Grip Power Strengthener
Description:
-
Used for progressive resistance hand therapy exercises.
Power web
Description:
-
Helps to strengthen and increase the range of motion in the hands after an injury or surgery.
-
Rebuilding strength, and regaining dexterity in the fingers, hands, and wrists.
Price: $88.63
To purchase, check this link: https://www.rehabmart.com/product/powerweb-and-powerweb-combo-44224.html
Silicone Power Web Grip
Description:
-
Improves dexterity, extension, and strengthening in hands, fingers, and thumbs.
Price: $65.99
To purchase, check this link: https://www.rehabmart.com/product/powerweb-flexgrip-44223.html
Thera-band
Description:
-
Used to strengthen Upper muscles
-
Each strength level is paired with a unique color for easy identification
Price: $32.65
To purchase, check this link: https://www.rehabmart.com/product/theraband-exercise-bands1-35056.html
Weighted Balls
Price: $19.99
Pegs and pegboard
Description:
-
Helps to improve cognitive skills: color recognition, math skills, vocabulary, and visual perceptual skills.
-
Helps to improve physical skills: hand/eye coordination, grasping skills, placement coordination skills, and dexterity.
Price: $116.72
To purchase, check this link: https://www.rehabmart.com/product/pegboard-with-round-pegs-9443.html
Ring Tree
Description:
-
It helps to improve ROM and coordination.
Price: $640.55
To purchase, check this link: https://www.rehabmart.com/product/ring-trees-21801.html
Inclined Bilateral Sander
Price: $615.66
Inclined Bilateral Shoulder Ladder
Description:
-
It helps to increase strength and range of motion.
Price: $326.47
To purchase, check this link: https://www.rehabmart.com/product/shoulder-exercise-ladder-14617.html
Sensory Box
Description:
-
Different sensory textures used to improve sensation
Dressing Board
Description:
-
Targets a variety of interests. Supports early dressing skills, hand-eye coordination and fine motor development. Ideal for special needs.
Price: $19
To purchase, check this link: https://www.amazon.com/Excellerations-Skills-Dressing-Boards-Pack/dp/B01I0E4QSE



-
Trigeminal Neuralgia. Available from: https://www.healthline.com/health/trigeminal-neuralgia#symptoms (Accessed 29 September 2020)
-
Hillis AE. Neurobiology of unilateral spatial neglect. The neuroscientist. 2006 Apr;12(2):153-63.fckLRDOI: 10.1177/1073858405284257
-
Menon A, Korner-Bitensky N. Evaluating unilateral spatial neglect post stroke: Working your way through the maze of assessment choices. Topics in stroke rehabilitation. 2004 Jul 1;11(3):41-66. DOI: http://dx.doi.org/10.1310/KQWL-3HQL-4KNM-5F4U
-
Plummer P, Morris ME, Dunai J. Assessment of unilateral neglect. (Update). Physical Therapy. 2003, August; 83(8): 732-740. DOI: https://doi.org/10.1093/ptj/83.8.732